
INTERNATIONAL COUNCIL OF NURSES
GUIDELINES
ON ADVANCED
PRACTICE NURSING
2020
Cover photo: The Twin Bridges Nurse Practitioner
All rights, including translation into other languages, reserved. No part of this publication may be reproduced in print,
by photostatic means or in any other manner, or stored in a retrieval system, or transmitted in any form, or sold
without the express written permission of the International Council of Nurses. Short excerpts (under 300 words)
may be reproduced without authorisation, on condition that the source is indicated.
Copyright © 2020 by ICN - International Council of Nurses,
3, place Jean-Marteau, 1201 Geneva, Switzerland
ISBN: 978-92-95099-71-5
INTERNATIONAL COUNCIL OF NURSES
GUIDELINES
ON ADVANCED
PRACTICE NURSING
2020

2
Mary Wambui Mwaniki
2
3
AUTHORS
Lead Author
Madrean Schober, PhD, MSN, ANP, FAANP
President, Schober Global Healthcare Consulting
International Healthcare Consultants
New York, NY, USA
Contributing Authors
Daniela Lehwaldt, PhD, MSc, PGDipED, BNS
Deputy Chair, ICN NP/APN Network
Assistant Professor and International Liaison
School of Nursing and Human Sciences
Dublin City University, Republic of Ireland
Melanie Rogers, PhD
Chair, ICN NP/APN Network
Advanced Nurse Practitioner
University Teaching Fellow
University of Hudderseld, U.K.
Mary Steinke, DNP, APRN-BC, FNP-C
ICN NP/APN Core Steering Group
Liaison, Practice Subgroup
Director Family Nurse Practitioner Program
Indiana University-Kokomo, Indiana, USA
Sue Turale, RN, DEd, FACN, FACMHN
Editor/Consultant
International Council of Nurses
Geneva, Switzerland
Visiting Professor, Chiang Mai University,
Chiang Mai, Thailand
Joyce Pulcini, PhD, PNP-BC, FAAN, FAANP
Professor, George Washington University
School of Nursing
Washington, DC, USA
Josette Roussel, MSc, MEd, RN
Program Lead, Nursing Practice and Policy
Programs and Policy
Canadian Nurses Association
Ottawa, Canada
David Stewart, RN, BN, MHM
Associate Director, Nursing and Health Policy
International Council of Nurses
Geneva, Switzerland
4 5
ACKNOWLEDGEMENT
ICN would like to thank the following people who provided a preliminary review of the guidelines:
•
Fadwa Affara, Consultant, Edinburgh, Scotland
•
Fariba Al Darazi, Prior Regional Director of Nursing, WHO, Regional Ofce of the Eastern Mediterranean
Region, Bahrain
•
Majid Al-Maqbali, Directorate of Nursing, Ministry of Health, Oman
•
Michal Boyd, Nurse Practitioner/Professor, University of Auckland, New Zealand
•
Lenora Brace, President, Nurse Practitioner Association of Canada
•
Karen Brennan, Past President, Irish Association of Nurse Practitioners
•
Denise Bryant-Lukosius, Professor, McMaster University, Canadian Centre for APN Research
•
Jenny Carryer, Professor, Massey University, New Zealand
•
Sylvia Cassiani, Regional Advisor for Nursing, Pan American Health Organization
•
Irma H. de Hoop, Dutch Association of Nurse Practitioners, Netherlands
•
Christine Dufeld, Professor, University of Technology, Sydney, Australia
•
Pilar Espinoza, Director, Postgraduate, research and international affairs at the health care sciences faculty
of the San Sebastián University, Chile
•
Lisbeth Fagerstrom, Professor, University College of Southeast Norway
•
Glenn Gardner, Emeritus Professor, Queensland University of Technology, Australia
•
Nelouise Geyer, CEO, Nursing Education Association, Pretoria, South Africa
•
Susan Hassmiller, Senior Advisor for Nursing, Robert Wood Johnson Foundation, USA
•
Heather Henry-McGrath, President, Jamaica Association of Nurse Practitioners, International
Ambassador-American Association of Nurse Practitioners
•
Simone Inkrot, Sabrina Pelz, Anne Schmitt, Christoph von Dach, APN/ANP Deutches Netzwerk G.E.V.,
Germany and Switzerland
•
Anna Jones, Senior Lecturer, School of Healthcare Sciences, College of Biomedical and Life Sciences,
Cardiff University, Wales
•
Elke Keinhath, Advanced Practice Nurse, APN/ANP Deutches Netzwerk G.E.V., Germany
•
Mabedi Kgositau, International Ambassador-American Association of Nurse Practitioners,
University of Botswana
•
Sue Kim, Professor, College of Nursing Yonsei University, South Korea
•
Karen Koh, Advanced Practice Nurse, National University Hospital, Singapore Nursing Board
•
Katrina Maclaine, Associate Professor, London South Bank University
•
Vanessa Maderal, Adjunct Professor, University of the Philippines
•
Donna McConnell, Lecturer in Nursing, Ulster University, Northern Ireland
•
Evelyn McElhinney, Senior lecturer, Programme Lead MSc Nursing: Advancing Professional Practice,
Glasgow Caledonian University, Scotland
•
Arwa Oweis, Regional Advisor for Nursing, WHO, Regional Ofce of the Eastern Mediterranean Region,
Cairo, Egypt
•
Jeroen Peters, Program Director, Nimigen University, Netherlands
•
Andrew Scanlon, Associate Professor, Montclair University, Australia
•
Bongi Sibanda, Advanced Nurse Practitioner, Anglophone Africa APN Coalition Project, Zimbabwe
•
Anna Suutaria, Head of International Affairs, Finnish Nurses’ Association
•
Peter Ullmann, Chair, APN/ANP Deutsches Netzwerk G.E.V., Germany
•
Zhou Wentao, Director, MScN Programme, National University of Singapore
•
Kathy Wheeler, Co-chair International Committee, American Association of Nurse Practitioners
•
Frances Wong, Professor, Hong Kong Polytechnic University
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
4 5
TABLE OF CONTENTS
List of Tables/Figures .............................................................................................................................................6
Glossary of terms ...................................................................................................................................................6
Foreword .................................................................................................................................................................7
Purpose of the ICN APN Guidelines .....................................................................................................................8
Abstract ...................................................................................................................................................................8
Chapter One: Advanced Practice Nursing ...........................................................................................................9
1.1 Introduction ..............................................................................................................................................9
1.2 Assumptions about Advanced Practice Nursing ..................................................................................9
1.3 Advanced Practice Nursing Characteristics .......................................................................................10
1.4 Country Issues that Shape Development of Advanced Practice Nursing ....................................... 11
Chapter Two: The Clinical Nurse Specialist (CNS) ............................................................................................12
2.1 ICN Position on the Clinical Nurse Specialist .....................................................................................12
2.2 Background of the Clinical Nurse Specialist ......................................................................................12
2.3 Description of the Clinical Nurse Specialist........................................................................................13
2.4 Clinical Nurse Specialist Scope of Practice ........................................................................................13
2.5 Education for the Clinical Nurse Specialist ........................................................................................14
2.6 Establishing a Professional Standard for the Clinical Nurse Specialist ..........................................14
2.7 Clinical Nurse Specialists’ Contributions to Healthcare Services ....................................................15
2.8 Differentiating a Specialised Nurse and a Clinical Nurse Specialist ................................................15
Chapter Three: The Nurse Practitioner ..............................................................................................................18
3.1 ICN Position on the Nurse Practitioner ................................................................................................18
3.2 Background of the Nurse Practitioner .................................................................................................18
3.3 Description of the Nurse Practitioner .................................................................................................18
3.4 Nurse Practitioner Scope of Practice...................................................................................................18
3.5 Nurse Practitioner Education ...............................................................................................................20
3.6 Establishing a Professional Standard for the Nurse Practitioner .....................................................21
3.7 Nurse Practitioner Contributions to Healthcare Services..................................................................21
Chapter Four: Distinguishing the Clinical Nurse Specialist and the Nurse Practitioner ...............................22
4.1 ICN Position on the Clarication of Advanced Nursing Designations ............................................23
References ............................................................................................................................................................27
Appendices ...........................................................................................................................................................33
Appendix 1: Credentialing Terminology ......................................................................................................33
Appendix 2: The International Context and Country Examples of the CNS .............................................33
Appendix 3: The International Context and Country Examples of the NP ................................................35
Appendix 4: Country exemplars of adaptations or variations of CNS and NP .........................................38
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
6
LIST OF TABLES/FIGURES
Table 1: Characteristics delineating Clinical Nurse Specialist practice
Table 2: Differentiating a Specialised Nurse and a Clinical Nurse Specialist
Table 3: Characteristics of Clinical Nurse Specialists and Nurse Practitioners
Table 4: Similarities between Clinical Nurse Specialists and Nurse Practitioners
Table 5: Differentiating the Clinical Nurse Specialist and the Nurse Practitioner
Figure 1: Progression from Generalist Nurse to Clinical Nurse Specialist
Figure 2: Distinction between Clinical Nurse Specialist and Nurse Practitioner
GLOSSARY OF TERMS
Advanced Nursing Practice (ANP)
Advanced Nursing Practice is a eld of nursing that
extends and expands the boundaries of nursing’s
scope of practice, contributes to nursing knowledge
and promotes advancement of the profession (RNABC
Policy Statement, 2001). ANP is ‘characterised by the
integration and application of a broad range of theoret-
ical and evidence-based knowledge that occurs as part
of graduate nursing education’ (ANA, 2010 as cited in
Hamric & Tracy, 2019, p. 63).
Advanced Practice Nurse (APN)
An Advanced Practice Nurse (APN) is a generalist or
specialised nurse who has acquired, through additional
graduate education (minimum of a master’s degree),
the expert knowledge base, complex decision-making
skills and clinical competencies for Advanced Nursing
Practice, the characteristics of which are shaped by
the context in which they are credentialed to practice
(adapted from ICN, 2008). The two most commonly
identied APN roles are CNS and NP.
Advanced Practice Nursing (APN)
Advanced Practice Nursing, as referred to in this paper,
is viewed as advanced nursing interventions that inu-
ence clinical healthcare outcomes for individuals,
fam ilies and diverse populations. Advanced Practice
Nursing is based on graduate education and prepar-
ation along with the specication of central criteria and
core competencies for practice (AACN, 2004, 2006,
2015; Hamric & Tracy, 2019).
Advanced Practice Registered Nurse (APRN)
APRN, as used in the USA, is the title given to a nurse
who has met education and certication requirements
and obtained a license to practice as an APRN in one
of four APRN roles: certied registered nurse anesthe-
tist (CRNA), certied nurse-midwife (CNM), Clinical
Nurse Specialist (CNS), and certied Nurse Practitioner
(CNP) (APRN Consensus Model, 2008).
Clinical Nurse Specialist (CNS)
A Clinical Nurse Specialist is an Advanced Practice
Nurse who provides expert clinical advice and care
based on established diagnoses in specialised clin-
ic al elds of practice along with a systems approach in
practicing as a member of the healthcare team.
Nurse Practitioner (NP)
A Nurse Practitioner is an Advanced Practice Nurse
who integrates clinical skills associated with nursing
and medicine in order to assess, diagnose and man-
age patients in primary healthcare (PHC) settings and
acute care populations as well as ongoing care for
popu lations with chronic illness.
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
6 7
FOREWORD
2020 has been named The International Year of the
Nurse and Midwife by the World Health Organization. It
celebrates both the professionals who provide a broad
range of essential health services to people every-
where as well as the bicentenary of the birth of Florence
Nightingale. However, the International Council of
Nurses (ICN) recognises that this year needs to be
more than just a celebration. It needs to be a time of
action and commitment by governments, health sys-
tems and the public to support the capacity, capability
and empowerment of the nursing profession to meet the
growing demands and health needs of individuals and
communities. Without the nursing profession, millions
of people around the world will not be able to access
quality, safe and affordable healthcare services. As the
largest group of healthcare workers providing the vast
majority of care, particularly in the primary care setting,
it is not surprising that the nursing workforce investment
can yield signicant improvement in patient outcomes.
Throughout history, we can see the continual evolution
of the nursing profession in order to address the health,
societal and person-centred care challenges.
It is for this reason, that as the global voice of nursing,
ICN has been calling for investment in nursing, and in
particular APN, to address global health challenges. As
a Commissioner on the WHO High Level Commission
on Noncommunicable Diseases (NCDs), the ICN
President witnessed the global community wrestle with
solutions to address the need to reduce mortality from
NCDs by 30% by 2030. What became clear was that
the status quo cannot continue and that governments
need to reorient their health systems and support
the health workforce, particularly APNs, to effectively
respond to promotion, prevention and management
of disease. This is echoed in the Astana Declaration
with the visionary pursuit of achieving Health for All
through Primary Health Care. The foundation for this
is nurses working to their full scope of practice. We
boldly declare, that APNs are an effective and efcient
resource to address the challenges of accessible, safe
and affordable health care.
This is clearly evident in Advanced Practice Nursing
(APN). Whilst this appears to be a relatively recent con-
cept, distinct patterns can be seen in the transition of
specialty practice into Advanced Practice Nursing over
the last 100 years. (Hanson & Hamric 2003)
Over this time there has been growing demand for APN
globally; however, many countries are in different stages
of development of these roles as part of the nursing
workforce. In addition, many APN positions have devel-
oped on an ad-hoc basis with varying responsibilities,
roles and nomenclature. The scope of practice is often
diverse and heterogenous across global regions. Often
pathways to entry and practice boundaries can be
blurred, poorly understood and sometimes contested.
This has led to confusion amongst policy makers,
health professionals and the public at large.
To seize the richness and opportunities afforded by
Advanced Practice Nursing, it is important that the pro-
fession provide clear guidance and direction. ICN has
been a leader in the development of the profession-
alisation of nursing since its very beginning in 1899.
It has provided guidance on a range of topics related
to nursing including the most widely used denition of
APN to date.
ICN is seeking to build on this work through the release
of these new guidelines on Advanced Practice Nursing.
Undertaken with the leadership support of the ICN
APN/NP Network, these guidelines have undergone an
extremely rigorous and robust global consultation pro-
cess. They aim to support the current and future devel-
opment of APN across countries in order to improve the
quality of service that our profession offers to individu-
als and communities.
Our hope is that through the development of these
guidelines, some of the barriers and walls that have hin-
dered the nursing profession can be torn down. These
guidelines will hopefully support the profession, enable
a clearer understanding and assist in the continual evo-
lution of APN. People around the world have the right
to quality, safe and affordable healthcare. Advanced
Practice Nurses are one of the solutions to making this
happen.
Annette Kennedy Howard Catton
ICN President ICN Chief Executive Ofcer

8
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
8
Mary Wambui Mwaniki
PURPOSE OF THE ICN APN GUIDELINES
The purpose of these guidelines is to facilitate a com-
mon understanding of Advanced Practice Nursing and
the Advanced Practice Nurse (APN) for the public,
governments, healthcare professionals, policy makers,
educators and the nursing profession. It is envisioned
that the work will support these stakeholders to develop
policies, frameworks and strategies supportive of an
Advanced Practice Nursing initiative. Those countries
that have implemented the APN role can review their
current state of Advanced Practice Nursing against
these recommended guidelines. This will support con-
sistency and clarity of Advanced Practice Nursing inter-
nationally and enable further development of APN roles
to meet the healthcare needs of individuals and com-
munities. This work is also important to the progres-
sion of research in this eld of nursing both within and
across countries.
It is recognised that the identication and context of
Advanced Practice Nursing varies in different parts of
the world. It is also acknowledged that the profession
is dynamic with changes to education, regulation and
nursing practice as it seeks to respond to healthcare
needs and changes to provision of healthcare services.
However, these guidelines provide common principles
and practical examples of international best practice.
ABSTRACT
In order to meet changing global population needs and
consumer expectations, healthcare systems worldwide
are under transformation and face restructuring. As
systems adapt and shift their emphasis in response to
the disparate requests for healthcare services, oppor-
tunities emerge for nurses, especially the APN, to meet
these demands and unmet needs (Bryant-Lukosius et
al. 2017; Carryer et al. 2018; Cassiani & Zug 2014;
Cooper & Docherty 2018; Hill et al. 2017; Maier et
al. 2017).
In 2002, the International Council of Nurses (ICN) pro-
vided an ofcial position on Advanced Practice Nursing
(ICN 2008a). Since that time, worldwide development
has increased signicantly and simultaneously this
eld of nursing has matured. ICN felt that a review of
its position was needed to assess the relevance of the
denition and characteristics offered in 2002. This guid-
ance paper denes diverse elements such as assump-
tions and core components of the APN. The attributes
and descriptors presented in this paper are intended
to promote a common vision to continue to enable a
greater understanding by the international nursing and
healthcare communities for the development of roles
commonly identied as Clinical Nurse Specialist (CNS)
and Nurse Practitioner (NP).

8
CHAPTER ONE: ADVANCED PRACTICE NURSING
98
CHAPTER ONE
ADVANCED PRACTICE NURSING
1.1 Introduction
1 In this paper, the emphasis is on the characteristics and professional standard of the CNS. The title of CNS is used to represent the role or level of nursing
as it is a widely identied category of Advanced Practice Nursing worldwide.
2 As per ICN’s denition of a nurse, the nurse is a person who has completed a programme of basic, generalised nursing education and is authorised by the
appropriate regulatory authority to practice nursing in his/her own country. https://www.icn.ch/nursing-policy/nursing-denitions
Advanced Practice Nursing, as discussed in this paper,
refers to enhanced and expanded healthcare ser-
vices and interventions provided by nurses who, in an
advanced capacity, inuence clinical healthcare out-
comes and provide direct healthcare services to indi-
viduals, families and communities (CNA 2019; Hamric
& Tracy 2019). An Advanced Practice Nurse (APN) is
one who has acquired, through additional education,
the expert knowledge base, complex decision-making
skills and clinical competencies for expanded nursing
practice, the characteristics of which are shaped by the
context in which they are credentialed to practice (ICN
2008a). The Clinical Nurse Specialist (CNS)
1
and Nurse
Practitioner (NP) are two types of APNs most frequently
identied internationally (APRN 2008; Begley 2010;
Carryer et al 2018; CNA 2019; Finnish Nurses
Association 2016; Maier et al. 2017, Miranda Neto
et al. 2018).
This guidance paper begins by providing overarching
assumptions of Advanced Practice Nursing. In addition,
core elements of the CNS and NP are presented in
Chapters Two and Three, together with ICN’s positions
on these nursing roles. In order to facilitate dialogue to
distinguish two types of APNs (CNSs and NPs), prac-
tice characteristics of the CNS and NP are presented
and differentiated in Chapter 4. Country exemplars pro-
vided in the Appendices depict the diversity of CNS and
NP practice.
1.2 Assumptions about Advanced Practice Nursing
The following assumptions represent the nurse who is
prepared at an advanced educational level and then
achieves recognition as an APN (CNS or NP). These
statements provide a foundation for the APN and a
source for international consideration when trying to
understand Advanced Practice Nursing, regardless of
work setting or focus of practice. All APNs:
•
are practitioners of nursing, providing safe
and competent patient care
•
have their foundation in nursing education
•
have roles or levels of practice which require formal
education beyond the preparation of the generalist
2
nurse (minimum required entry level
is a master’s degree)
•
have roles or levels of practice with increased levels
of competency and capability that are measurable,
beyond that of a generalist nurse
•
have acquired the ability to explain and apply
the theoretical, empirical, ethical, legal, care
giving, and professional development required
for Advanced Practice Nursing
•
have dened APN competencies and standards
which are periodically reviewed for maintaining
currency in practice, and
•
are inuenced by the global, social, political,
economic and technological milieu.
(Adapted from ICN 2008a)
The degree and range of judgement, skill, knowledge,
responsibility, autonomy and accountability broadens
and takes on an additionally extensive range between
the preparation of a generalist nurse and that of the
APN. This added breadth and further in-depth prac-
tice is achieved through experience in clinical practice,
additional education, and a master’s degree or beyond.
However, the core of the APN remains based within the
context of nursing and nursing principles (Adapted from
ICN 2008a).
Results from research conducted in Australia found that
nurses in the eld of Advanced Practice Nursing exhibit
patterns of practice that are different from other nurses
(Gardner et al, 2015). Using an Advanced Practice
Role Delineation tool based on the Strong Model of
Advanced Practice, ndings demonstrate the cap-
acity to clearly delineate and dene Advanced Practice
Nursing (Gardner et al, 2017). The signicance of this
research suggests that, from a healthcare workforce
perspective, it is possible to measure the level of nurs-
ing practice identied as Advanced Practice Nursing
and to more clearly identify these roles and positions.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
10
1.3 Advanced Practice Nursing Characteristics
Role characteristics can be viewed as features that
make Advanced Practice Nursing and the APN rec-
ognisable. Descriptions of the domains of education,
practice, research, leadership and professional regula-
tion provide guidance when making a clear distinction
between advanced versus generalist nursing practice.
While the core of APN practice is based on advanced
nursing education and knowledge, an overlap of expert-
ise may occur with other healthcare professionals. The
breadth and depth of autonomy associated with the
APN often arises within a broader and more extensive
range in community-based services such as primary
healthcare, ambulatory services and out-of- hospital set-
tings. The degree of autonomy may evolve or expand
over time as the concept of Advanced Practice Nursing
gains recognition.
The following sections provide guidelines for identifying
Advanced Practice Nursing:
Educational preparation
•
Educational preparation beyond that of a generalist
or specialised nurse education at a minimum
requirement of a full master’s degree programme
(master’s level modules taken as detached courses
do not meet this requirement). It is acknowledged
that, for some countries, the requirement of a
master’s degree may be an aspirational goal
as they strive to achieve this standard. Transitional
programmes and bridging courses can be dened
to progress to this standard.
•
Formal recognition of educational programmes
preparing nurses specically for Advanced
Practice Nursing (CNS or NP) (e.g. accreditation,
approval or authorisation by governmental
or nongovernmental agencies).
•
A formal system of credentialing linked to dened
educational qualications.
•
Even though some countries require clinical
experience for a nurse to enter an APN education
programme, no evidence was found to support
this requirement.
Nature of practice
•
A designated role or level of nursing that
has its focus on the provision of care, illness
prevention and cure based on direct and indirect
healthcare services at an advanced level,
including rehabilitative care and chronic disease
management. This is beyond the scope of practice
of a generalist or specialised nurse (see Section 2.3
for denitions of direct and indirect care).
•
The capability to manage full episodes of care
and complex healthcare problems including hard
to reach, vulnerable and at-risk populations.
•
The ability to integrate research (evidence informed
practice), education, leadership and clinical
management.
•
Extended and broader range of autonomy (varies
by country context and clinical setting).
•
Case-management (manages own case load
at an advanced level).
•
Advanced assessment, judgement, decision-making
and diagnostic reasoning skills.
•
Recognised advanced clinical competencies,
beyond the competencies of a generalist
or specialised nurse.
•
The ability to provide support and/or consultant
services to other healthcare professionals
emphasising professional collaboration.
•
Plans, coordinates, implements and evaluates
actions to enhance healthcare services
at an advanced level.
•
Recognised rst point of contact for clients
and families (commonly, but not exclusively,
in primary healthcare settings).
Regulatory mechanisms – Country specic
professional regulation and policies underpinning
APN practice:
•
Authority to diagnose
•
Authority to prescribe medications
•
Authority to order diagnostic testing and therapeutic
treatments
•
Authority to refer clients/patients to other services
and/or professionals
•
Authority to admit and discharge clients/patients
to hospital and other services
•
Ofcially recognised title(s) for nurses working
as APNs
•
Legislation to confer and protect the title(s)
(e.g. Clinical Nurse Specialist, Nurse Practitioner)
•
Legislation and policies from an authoritative
entity or some form of regulatory mechanism
explicit to APNs (e.g. certication, credentialing
or authorisation specic to country context)
(Adapted from ICN, 2008a)
The assumptions and characteristics for Advanced
Practice Nursing are viewed as inclusive and exible
to take into consideration variations in healthcare sys-
tems, regulatory mechanisms and nursing education in
individual countries. Over the years, Advanced Practice
Nursing and nursing globally have matured with the APN
seen as a clinical expert, with characteristics of the role
crosscutting other themes that include understanding
and inuencing the issues of governance, policy devel-
opment and clinical leadership (AANP 2015; CNA 2019;
Scottish Government 2008; NCNZ 2017a). Promotion
of leadership competencies and integration of research
knowledge and skills have increasingly become core
elements of education and role development along
with advanced clinical expertise. In the United Kingdom
(UK), all four countries use a four-pillars coordinated
approach encompassing clinical practice, leadership,
education and research. Clinical practice is viewed as
the main pillar to develop when faced with funding and
human resource issues (personal communication K.
Maclaine, March 2019).

10
CHAPTER ONE: ADVANCED PRACTICE NURSING
11
1.4 Country Issues that Shape Development of Advanced Practice Nursing
The fundamental level of nursing practice and access
to an adequate level of nursing education that exists
in a country shapes the potential for introducing and
developing Advanced Practice Nursing. Launching an
Advanced Practice Nursing initiative is inuenced by the
professional status of nursing in the country and its ability
to introduce a new role or level of nursing. The prom-
inence and maturity of nursing can be assessed by the
presence of other nursing specialties, levels of nursing
education, policies specic to nurses, extent of nursing
research and nursing leadership (Schober 2016).
It is acknowledged that in countries where generalised
nursing education is progressing and the country con-
text is considering development of a master’s degree
education for Advanced Practice Nursing, that transition
programmes or bridging courses can be developed to
prepare generalist or specialised nurses for CNS or NP
roles. Transition curricula have the potential for lling in
educational gaps as nursing education in the country
evolves toward the master’s degree requirement.
In addition, it is recognised that there are countries that
have clear career tracks or career ladders and grading
(e.g. banding) systems in place for nursing role titles,
descriptions, credentials, hiring practices and policies.
These grading systems or level of roles will impact on
implementation of the APN (CNS or NP) as the grading
system stipulates a certain level of education and years
of experience at each level, including roles at advanced
levels. Such a grading system is likely to ensure that
nurses working in a specic grade perform at a more
consistent level since they would be viewed to have
similar education and experience. Protected role titles
with clear credentialing requirements help ensure con-
sistent role implementation at the desired level.
Most importantly, these guidelines emphasise that the
APN is fundamentally a nursing role, built on nursing
principles aiming to provide the optimal capacity to
enhance and maximise comprehensive healthcare
services. The APN is not seen as in competition with
other healthcare professionals, nor is the adoption of
the domains of other healthcare providers viewed as
the core of APN practice.
Chioma

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
12
CHAPTER TWO
THE CLINICAL NURSE SPECIALIST (CNS)
3
The Clinical Nurse Specialist (CNS) is one commonly identied category of Advanced Practice Nursing (APRN &
NCSBN 2008; Barton & Allan 2015; CNA 2019; Maier et al. 2017; Tracy & O’Grady 2019). This section describes
the historical background of the CNS, denes the role and explains how a scope of practice and education pro-
vide the foundation for the CNS. In addition, credentialing and regulatory mechanisms are dened as well as their
importance in establishing the identity and professional standard for CNSs.
2.1 ICN Position on the Clinical Nurse Specialist
3 It is acknowledged there are countries with Clinical Nurse Consultants (CNC) whose practice is viewed to be consistent with CNS practice
(Bryant-Lukosius & Wong, 2019; Carryer et al. 2018; Gardner et al. 2013; Gardner et al. 2016). The use of CNC is country specic and at times
used interchangeably with CNS, however, this guidance paper focuses on identifying the CNS.
The CNS is a nurse who has completed a master’s
degree programme specic to CNS practice. The CNS
provides healthcare services based on advanced spe-
cialised expertise when caring for complex and vulner-
able patients or populations. In addition, nurses in this
capacity provide education and support for interdiscip-
linary staff and facilitate change and innovation in
healthcare systems. The emphasis of practice is on
advanced specialised nursing care and a systems
approach using a combination of the provision of direct
and indirect clinical services (see Section 2.3 for den-
itions of direct and indirect care). This prole of the CNS
is based on current evidence of the successful pres-
ence of the role in some countries; however, often the
CNS role is present but invisible in settings where these
nurses provide a valuable service. Further research is
needed to clearly identify the diversity of the settings
and countries where the CNS practices.
As healthcare reform worldwide continues to gain
momentum, there will be opportunities for nurses in
CNS practice to meet the unmet needs of varied popu-
lations and diverse healthcare settings. Crucial to taking
advantage of these possibilities is the need to improve
understanding of the CNS in the Advanced Practice
Nursing context. In order to grasp an increased appre-
ciation and comprehension of the CNS, the requirement
for title protection, graduate education (minimum mas-
ter’s degree), and an identiable scope of practice as
part of a credentialing process, is seen as optimal.
2.2 Background of the Clinical Nurse Specialist
The expanded role of nursing associated with a CNS
is not a recent phenomenon. The term ‘specialist’
emerged in the United States (USA) in the 19
th
and
early 20
th
Centuries as more postgraduate courses in
specic areas of nursing practice became avail able
(Barton & East 2015; Cockerham & Keeling 2014;
Keeling & Bigbee 2005). The origin of the CNS emerged
from an identied need for specialty practices (Chan &
Cartwright 2014). Psychiatric Clinical Nurse Specialists
along with nurse anesthetists and nurse midwives led
the way. The growth of hospitals in the 1940s as well
as the development of medical specialties and technol-
ogies further stimulated the evolution of the CNS.
These nurses were considered to practice at a higher
degree of specialisation than that already present in
nursing and are viewed as the originators of the current
CNS role. Even though there has been an evolution of
role development internationally over the years, CNS
origins were seen to lie comfortably within the tradition-
ally understood domain of nursing practice and thus the
CNS was able to progress unopposed (Barton & East
2015).
Similarly, in Canada, CNSs rst emerged in the 1970s
as provision of healthcare services grew more com-
plex. The concept of the role was to provide clinical
consult ation, guidance and leadership to nursing staff
managing complex and specialised healthcare in order
to improve the quality of care and to promote evidence-
informed practice. CNSs were focused on complex patient
care and healthcare systems issues which required
improvements. The result of the CNS presence was
measurable positive outcomes for the populations they
cared for (CNA 2019).
The following reasons for the conception of the CNS
role were proposed by Chan and Cartwright (2014: 359):
•
Provide direct care to patients with complex
diseases or conditions
•
Improve patient care by developing the clinical skills
and judgement of staff nurses
•
Retain nurses who are experts in clinical practice
The CNS role has developed over time, becoming
more exible and responsive to population healthcare
needs and healthcare environments. For example, in
Sub-Saharan Africa, the CNS is well developed, par-
ticularly in the progress made in HIV management and
prevention for these vulnerable populations (personal
communication, March 2019, B. Sibanda). The funda-
mental strength of the CNS role is in providing complex
specialty care while improving the quality of healthcare
delivery through a systems approach. The multifa ceted
CNS prole, in addition to direct patient care in a clin-
ical specialty, includes indirect care through educa-
tion, research and support of other nurses as well as
healthcare staff, provides leadership to specialty prac-
tice programme development and facilitates change
and innovation in healthcare systems (Lewandowski &
Adamle 2009).

12
CHAPTER TWO: THE CLINICAL NURSE SPECIALIST (CNS)
13
2.3 Description of the Clinical Nurse Specialist
The CNS is a nurse with advanced nursing knowledge
and skills, educated beyond the level of a generalist
or specialised nurse, in making complex decisions in
a clinical specialty and utilising a systems approach to
inuence optimal care in healthcare organisations.
While CNSs were originally introduced in hospitals
(Delamaire & LaFortune 2010), the role has evolved
to provide specialised care for patients with com-
plex and chronic conditions in outpatient, emergency
department, home, community and long-term care
settings (Bryant-Lukosius & Wong 2019; Kirkpatrick
et al. 2013). Commonly, the provision of healthcare
services by a CNS includes the combination of direct
and indirect healthcare services (refer to Section 2.3)
based on nursing principles and a systems perspective
(CNA 2014; NACNS 2004; NCNM 2007). It is acknow-
ledged that indirect services of the CNS are highly val-
ued along with direct clinical care and should be taken
into consideration when dening scope of practice.
Although nurses who practice in various specialties
(e.g. intensive care unit, theatre/surgery, palliative care,
wound care, neonatal, gerontology) may consider them-
selves at times to be specialised nurses, the designated
CNS has a broader and extended range of accountabil-
ity and responsibility for improvements in the healthcare
delivery system, including an advanced level clinical
specialty focus. Based on postgraduate education at
a minimum of a master’s or doctoral degree, the CNS
acquires additional in-depth knowledge, critical thinking
and decision-making skills that provide the foundation
for an advanced level of practice and decision making.
2.4 Clinical Nurse Specialist Scope of Practice
The scope of practice for the CNS extends beyond the
generalist and specialised nurse in terms of advanced
expertise, role functions, mastery of a specic specialty
with an increased and expanded level of practice that
includes broader and more in-depth accountability. The
scope of practice reects a sophisticated core body of
practical, theoretical and empiric nursing and health-
care knowledge. CNSs evaluate disease patterns,
technological advances, environmental conditions and
political inuences. In addition, they interpret nursing’s
professional responsibility to serve the public’s need for
nursing services. CNSs function as expert clinicians in
a specialty and are leaders in advancing nursing prac-
tice by teaching, mentoring, consulting and ensuring
nursing practice is evidence-based/evidence-informed.
Table 1: Characteristics delineating Clinical Nurse Specialist Practice
THE FOLLOWING CHARACTERISTICS, IN VARYING COMBINATIONS, DELINEATE CNS PRACTICE
• Clinical Nurse Specialists (CNSs) are professional nurses with a graduate level preparation
(master’s or doctoral degree).
• CNSs are expert clinicians who provide direct clinical care in a specialised area of nursing practice.
Specialty practice may be dened by population (e.g. pediatrics, geriatrics, women’s health); clinical
setting (e.g. critical care, emergency); a disease/medical subspecialty (e.g. oncology, diabetes);
type of care (psychiatric, rehabilitation); or type of problem (e.g. pain, wound, incontinence).
• Clinical practice for a specialty population includes health promotion, risk reduction, and management
of symptoms and functional problems related to disease and illness.
• CNSs provide direct care to patients and families, which may include diagnosis and treatment of disease.
• CNSs practice patient/family centred care that emphasises strengths and wellness over disease or decit.
• CNSs inuence nursing practice outcomes by leading and supporting nurses to provide scientically
grounded, evidence-based care.
• CNSs implement improvements in the healthcare delivery system (indirect care) and translate high-quality
research evidence into clinical practice to improve clinical and scal outcomes.
• CNSs participate in the conduct of research to generate knowledge for practice.
• CNSs design, implement and evaluate programmes of care and programmes of research that address
common problems for specialty populations. (Fulton & Holly April 2018)
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
14
In dening the scope of practice for the CNS, identi-
cation of core competencies includes levels of direct
and indirect nursing care. These levels of care include
assisting other nurses and health professionals in
establishing and meeting healthcare goals of individ-
uals and a diverse population of patients (CNA 2014;
NACNS 2004).
•
Direct Care involves direct interaction with patients,
families and groups of patients to promote health
or well-being and improve quality of life. Direct care:
•
integrates advanced knowledge of wellness,
illness, self-care, disease and medical
therapeutics in a holistic assessment of people
while focusing on the nursing diagnosis
of symptoms, functional problems and risk
behaviours that have etiologies requiring nursing
interventions to prevent, maintain or alleviate;
•
utilises assessment data, research and theoretical
knowledge to design, implement and evaluate
nursing interventions that integrate delegated
medical treatments as needed; and
•
prescribes or orders therapeutic interventions.
•
Indirect Care involves indirect provision
of care through activities that inuence the care
of patients, but do not involve direct engagement
with populations. Examples include developing
evidence-based/evidence-informed guidelines
or protocols for care and staff development
activities. A CNS providing indirect care:
•
serves as a consultant to other nurses
and healthcare professionals in managing
highly complex patient care problems
and in achieving quality, cost-effective outcomes
for populations across healthcare settings;
•
provides leadership in appropriate use
of research/evidence in practice innovations
to improve healthcare services;
•
develops, plans and directs programmes of care
for individuals and populations and provides
direction to nursing personnel and others
in these programmes of care;
•
evaluates patient outcomes and
cost-effectiveness of care to identify needs
for practice improvements within the clinical
specialty or programme; and
•
serves as a leader of multidisciplinary groups in
designing and implementing alternative solutions
to patient care issues across the continuum
of care. (CNA 2014; NACNS 2004)
2.5 Education for the Clinical Nurse Specialist
A graduate programme (master’s or doctoral degree)
specifically identified for CNS education from an
accredited school/university or department of nursing
is viewed as important for providing the necessary
preparation for the CNS. The goal of the educational
programme is to prepare the nurse to think critically
and abstractly at an advanced level in order to assess
and treat patients/families/populations as well as to
teach and support other nurses and healthcare profes-
sionals in complex clinical situations. The educational
programme prepares the CNS to use and integrate
research into clinical practice, regardless of setting or
patient population.
Educational preparation is built on the educational foun-
dation for the generalised or specialised nurse in the
country in which the CNS will practice. In support of a
minimum standard for master’s level education, three
Canadian studies have demonstrated that self- identied
CNSs who have completed a master’s degree are more
likely to implement all recognised domains of Advanced
Nursing Practice compared to those who are not pre-
pared at the master’s level (Bryant-Lukosius et al. 2018;
Kilpatrick et al. 2013; Schreiber et al. 2005). Not only
do these studies demonstrate that graduate-prepared
CNSs function differently than the BScN-prepared
nurse, but they also show that the CNSs improve health
outcomes at the population health level, and further
contribute to innovation and improvement of the unit,
organisation and systems levels to improve access to
and quality of nursing and healthcare services.
2.6 Establishing a Professional Standard for the Clinical Nurse Specialist
In addition to following the professional standard for the
generalist nurse, the CNS is responsible for meeting
the standard or dened competencies for advanced
practice such as:
•
Providing nursing services beyond the level
of a generalist or specialised nurse that are
within the scope of the designated specialty
eld of advanced practice for which
he or she is educationally prepared
•
Recognising limits of knowledge and competence
by consulting with or referral of patients/populations
to other healthcare professionals when appropriate
•
Adhering to the ethical standards articulated
by the profession for APNs
A professional standard denes the boundaries and
essential elements of practice and connects the CNS
to the expected quality and competence for the role
or level of practice through the description of required
components of care. The identied criteria for the pro-
fessional standard serve to establish rules, conditions
and performance requirements that focus on the pro-
cesses of care delivery.

14
CHAPTER TWO: THE CLINICAL NURSE SPECIALIST (CNS)
15
Credentialing and Regulation
for the Clinical Nurse Specialist
Recognition to practice as a CNS requires submis-
sion of evidence to an authoritative credentialing entity
(governmental or nongovernmental agency) of suc-
cessful completion of a master’s or doctoral degree
programme in a designated clinical specialty from an
accredited school or department of nursing. The focus
of the educational programme must be specically
identied as preparation of nurses to practice as CNSs.
Continuing recognition to practice is concurrent with
renewal of the generalist nursing licence and all appro-
priate professional regulation for CNS practice in the
state, province or country in which the CNS practices.
In some countries, prescriptive authority is integral to
the CNS role and is governed by country, state or prov-
ince regulations based on the clinical area in which he
or she practices. In addition to completion of a CNS
educational programme, there may be a stipulation that
the CNS must complete an additional certication or
4 In its Regulation Series, ICN provides a Nursing Care Continuum Framework & Competencies (ICN 2008b) and denes the specialised nurse as a nurse
prepared beyond the level of a generalist nurse, authorised to practice as a specialist in a branch of the nursing eld.
credentialing process in order to demonstrate excel-
lence in practice and competence in the designated
eld or specialty in which he or she will practice. This
requirement is sensitive to the environment in which the
CNS initiative emerges and is developed.
Policies that provide title protection and clear creden-
tialing are important for role recognition and clarity.
Regulated title protection for the CNS is considered opti-
mal (CNA 2019). Studies on Advanced Practice Nursing
have found that countries in which titles and scope of
practice are regulated generally achieve greater role
clarity, recognition and acceptance by the consumer
and other healthcare professionals (Maier et al. 2017;
Donald et al. 2010). It is acknowledged that this is
especially important for CNSs as these nurses seek to
achieve increased visibility in demonstrating the import-
ance of their roles in healthcare systems worldwide.
Refer to Appendix 1 for Credentialing Terminology.
2.7 Clinical Nurse Specialists’ Contributions to Healthcare Services
Evidence from systematic literature reviews giving
examples of benecial outcomes of care provided by
a CNS include:
•
Improved access to supportive care through
collaborative case management to assess and
manage risks and complications, plan and
coordinate care, and monitoring and evaluation
to advocate for health and social services
that best meet patient/client needs
•
Enhanced quality of life, increased survival
rates, lower complication rates and improved
physical, functional and psychological well-being
of populations with complex acute or chronic
conditions
•
Improved quality of care
•
Improvement in health promotion
•
Contribution to the recruitment and retention
of nurses in the healthcare workforce
•
Decreased lengths of stay in hospital and reduced
hospital re-admissions and emergency department
visits
•
Reduction in medication errors in hospital wards
and operating rooms
(Brown-Brumeld & DeLeon 2010; Bryant-Lukosius
et al. 2015a; Bryant-Lukosius et al. 2015b;
Bryant-Lukosius & Martin-Misener. 2016;
Cook et al. 2015; Flanders & Clark 2010;
Kilpatrick et al. 2014)
The multifaceted nature of CNS practice and the vari-
ability by which these nurses adapt to diverse requests
has created confusion about what CNSs do. As a
result, this confusion challenges understanding of the
impact of the CNS role on clinical outcomes (Chan &
Cartwright 2014). Further collaborative research is
needed to improve this gap in knowledge. In addition,
CNSs and nurse leaders need to be more proactive in
articulating to healthcare funders and decision-makers
the value-added contributions of CNSs; this includes
their alignment with policy priorities for health system
improvement and contribution to healthcare policy
and decision-makers in achieving positive outcomes
(Bryant-Lukosius & Martin-Misener 2016).
2.8 Differentiating a Specialised Nurse
4
and a Clinical Nurse Specialist
It is acknowledged that in some countries there are
nurses with extensive experience and expertise in a
specialty who are not educated through a university
or post-graduate degree. For example, in Chile, the
specialised nurse is a highly recognised and valued
professional of the healthcare team and the healthcare
organisation, identied as such based on completion
of short courses or incidental training in addition to
extensive experience. It is envisioned that in the future,
a specialised nurse in Chile could proceed to enter a
CNS master’s degree educational programme in order
to promote change, implement system improvements
and enhance quality of care in clinical settings (per-
sonal communication, Pilar Espinoza, March 2019).
In its regional guide for the development of special-
ised nursing practice, the World Health Organization
Eastern Mediterranean Regional Ofce (WHO-EMRO)
provides the following denition:
A specialist nurse holds a current license as a general-
ist nurse, and has successfully completed an education
programme that meets the prescribed standard for spe-
cialist nursing practice. The specialist nurse is author-
ised to function within a dened scope of practice in a
specied eld of nursing.
(WHO-EMRO 2018: 7)
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
16
One criterion for designating a specialty for nursing
practice stipulates that the specialty is ofcially rec-
ognised and supported by the health system in the
country. In addition, levels of specialist nursing practice
progress to an advanced level of specialisation such
as the CNS based on completion of a clinical master’s
degree in the area of specialisation, and using the title
Registered Advanced Practice Nurse with area of spe-
cialty indicated. For example, Registered Advanced
Practice Cardiac Nurse (WHO-EMRO 2018).
Similarly, the European Specialist Nurses Organization
(ESNO 2015) recommends development of compe-
tencies for the CNS to clarify the position and prac-
tice of this nurse in Europe. This recommendation
includes building a framework corresponding to the
features of the specialty in which the CNS will practice.
Identication of consistent qualications would enable
the CNS the possibility to move more easily within the
member states of Europe. Consistent with the guide-
lines in this paper, ESNO identies the CNS as an
APN, educated within a clinical specialty at a master’s,
post-master’s or doctoral level.
From the perspective of workforce development and
healthcare reform, it is understood that delivery of
healthcare services requires a range of personnel
and that there would be larger numbers of special-
ised nurses in staff positions versus CNSs. CNSs with
advanced clinical expertise and a graduate degree
(minimum of master’s degree) in a clinical specialty
function collaboratively within healthcare teams. They
use a systems approach to coordinate directives of
specialty care in addition to providing direct healthcare
services. Table 2 below is a useful tool to distinguish the
characteristics of the specialised nurse and the CNS.
Table 2: Differentiating a Specialised Nurse and a Clinical Nurse Specialist
AREA SPECIALISED NURSE CNS
Education Preparation beyond the level
of a generalist nurse
in a specialty.
Master’s degree or beyond
with a specialty focus.
Scope of Practice
Job Description
Performs identied activities
in a specialty in line with
personal level of prociency
and scope of practice.
Formulates a care plan
in a specialty with identied care
outcomes based on nursing
diagnoses, and ndings
from a nursing and health
assessment, inputs from other
health team members
and nursing practice standards.
In addition to advanced
specialised direct clinical care,
formulates and mobilises
resources for coordinated
comprehensive care with
identied care outcomes.
This is based on CNS practice
standards, and informed
decisions about preventive,
diagnostic and therapeutic
interventions.
Delegates activities to other
healthcare personnel, according
to ability, level of preparation,
prociency and scope
of practice.
Advocates for and implements
policies and strategies from
a systems perspective to
establish positive practice
environments, including the use
of best practices in recruiting,
retaining and developing human
resources.
Professional Standard
& Regulation
Country standard for a licensed
generalist nurse in addition
to identied preparation
(experience and education)
as a specialised nurse.
Designated/protected CNS title
from a legislative or regulatory
agency. Preferred model is
transitioning to title protection if it
does not currently exist.

16
CHAPTER TWO: THE CLINICAL NURSE SPECIALIST (CNS)
17
Figure 1: Progression from Generalist Nurse to Clinical Nurse Specialist
Generalist nurse
9 Diploma/Bachelors
Degree
Specialized nurse
9 Extensive experience
9 Specialized clinical courses
or modules and/or
on the job training
Clinical Nurse Specialist
9 Master’s Degree
or higher with a specialty
focus
Figure 1 depicts the progression from that of a gen-
eralist nurse to a CNS and then educated in a CNS
specic master’s degree programme. This progression
provides recognition of the foundation of specialised
clinical expertise based on the foundation of a general-
ist nursing education. A generalist nurse may proceed
to enter a CNS programme directly if the candidate
meets national and academic criteria for CNS prep-
aration. Completion of a minimum of a master’s degree
provides enhanced professional as well as clinical cred-
ibility for the nurse, who progresses and distinguishes
themselves as a CNS. The additional education and
clinical expertise gained with an academic degree has
the potential to further assure quality of care for diverse
populations. Based on standardised and accredited
academic programmes, this level of professional devel-
opment is viewed as essential when seeking to deliver
optimal safe and high-quality healthcare by enhancing
academic rigor, scientic reasoning and critical thinking.
Refer to Appendix 2, p. 33 for country exemplars of the
Clinical Nurse Specialist.
Carolyn Jones

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
18
CHAPTER THREE
THE NURSE PRACTITIONER
The Nurse Practitioner (NP) is one commonly identied category of APN (APRN 2008; Barton & Allan 2015;
Maier et al. 2017; Tracy & O’Grady 2019). This chapter presents the ICN position on NP, portrays the historical
background, describes the NP concept and explains how a scope of practice and appropriate education provide
the foundation for clinical practice. In addition, this chapter denes credentialing and regulatory mechanisms and
discusses their importance in establishing NPs in a variety of settings.
3.1 ICN Position on the Nurse Practitioner
Narrative descriptions and research demonstrate the
effectiveness of NPs within a variety of healthcare
settings. The international momentum for NP ser-
vices is increasing, however several themes need to
be confronted and managed to successfully launch
and sustain an effective NP initiative. Title protection
and a well-developed scope of practice sensitive to a
country’s healthcare system(s) and culture are critical.
The scope of practice and identied competencies for
the NP require a sound educational foundation along
with supportive credentialing and regulatory processes.
Continued research to provide evidence of the value
of NPs in provision of healthcare services will continue
to be needed to support the legitimacy of NP practice.
3.2 Background of the Nurse Practitioner
The concept of the NP was initiated in 1965 in the USA
based on a public health model to provide primary health-
care (PHC) to children lacking access to healthcare ser-
vices. The role was based on a person-centred, holistic
approach to care with the addition of diagnostic, treat-
ment and management responsibilities previously limited
to physicians. However, it was distinct from the medical
model in that it focused also on prevention, health and
wellness, and patient education (Dunphy et al. 2019). In
the mid-1970s, Canada and Jamaica followed the USA’s
development, aiming to improve access to PHC for vul-
nerable populations in rural, remote and underserved
communities. In the 1980s in Botswana, as the country
responded to healthcare reform and population needs
of the country spiraled, a Family Nurse Practitioner role
was launched. This was followed by introduction of the
NP in the four countries of the UK in the late 1980s. In the
1990s and early 2000s, additional countries introduced
NPs with ICN and the international healthcare commu-
nity noting signicant increased interest and development
worldwide (Maier et al. 2017; Schober 2016).
Since its beginnings, the focus of the NP has evolved to
include general patient populations across the lifespan
in PHC as well as to meet the complex needs of acute
and critically ill patients. Enthusiasm for the NP concept
and trends toward increasing access to PHC services
indicate that growing numbers of NPs are working to
expand care in diverse settings; this includes ageing
populations and those with chronic conditions in ambu-
latory settings and home care (Bryant-Lukosius &
Wong, 2019; Kaasalainen et al. 2010; Maier et al. 2017;
Schober 2016).
The NP concept often develops out of healthcare needs
as well as perceived criteria by individual, practicing
nurses who envision the enhancement of healthcare
services that can be provided to diverse populations
by NPs (Steinke et al. 2017). As the NP concept has
evolved, comprehensive PHC remains a common
focus with a foundation for practice that continues to be
based on nursing principles.
3.3 Description of the Nurse Practitioner
NPs are generalist nurses who, after additional edu-
cation (minimum master’s degree for entry level), are
autonomous clinicians. They are educated to diag-
nose and treat conditions based on evidence-informed
guidelines that include nursing principles that focus on
treating the whole person rather than only the condi-
tion or disease. The level of practice autonomy and
accountability is determined by, and sensitive to, the
context of the country or setting and the regulatory
policies in which the NP practices. The NP brings a
comprehensive perspective to healthcare services by
blending clinical expertise in diagnosing and treating
health conditions, including prescribing medications,
and with an added emphasis on disease prevention
and health management. NP practice is commonly
identied by the patient population, such as family,
paediatric, adult- gerontological or women’s health,
and may be practiced in PHC or acute care settings
(AANP 2018; CNA 2018; NMBI 2017; RCN 2018;
Scottish Government 2008).
3.4 Nurse Practitioner Scope of Practice
A scope of practice for the NP refers to the range of
activities (procedures, actions, processes) that a NP is
legally permitted to perform. This scope of practice sets
parameters within which the NP may practice by den-
ing what the NP can do, which population can be seen
or treated, and under what circumstances the NP can
provide care. Furthermore, once dened, the scope of
practice and associated competencies are linked to the
designated title and form the foundation for develop-
ing appropriate education and a professional standard
(ANA 2015; AANP 2015; Schober 2016).
The scope of practice for the NP differs from that of
the generalist nurse in the level of accountability and
responsibility required to practice. Where the NP con-
cept is recognised, establishment of a scope of practice

18
CHAPTER THREE: THE NURSE PRACTITIONER
19
is one way of informing the public, administrators and
other healthcare professionals about the role in order to
differentiate the qualied NP from other clinicians who
are not adequately prepared for NP practice or have not
been authorised to practice in this capacity.
ICN position on the Nurse Practitioner scope
of practice
A scope of practice for the NP describes the range
of activities associated with recognised professional
responsibilities consistent with regulation and policy in
the setting(s) in which the NP practices. Understanding
the country/state/provincial context in which the NP will
practice is fundamental when dening a scope of practice
for NP provision of healthcare services. In addition, it is
essential that development of a scope of practice focuses
on the activities of an NP that underpins the more complex
knowledge and skill sets of NP practice. ICN takes the fol-
lowing position for a Nurse Practitioner Scope of Practice:
The Nurse Practitioner possesses advanced health
assessment, diagnostic and clinical management
skills that include pharmacology management
based on additional graduate education (minimum
standard master’s degree) and clinical education
that includes specied clinical practicum in order to
provide a range of healthcare services. The focus of
NP practice is expert direct clinical care, managing
healthcare needs of populations, individuals
and families, in PHC or acute care settings with
additional expertise in health promotion and disease
prevention. As a licensed and credentialed clinician,
the NP practices with a broader level of autonomy
beyond that of a generalist nurse, advanced in-depth
critical decision-making and works in collaboration
with other healthcare professionals. NP practice
may include but is not limited to the direct referral
of patients to other services and professionals. NP
practice includes integration of education, research
and leadership in conjunction with the emphasis on
direct advanced clinical care.
Examples of Nurse Practitioner scope of practice
from three countries
Each country where the NP is well developed needs a
robust scope of practice. Three examples of NP scopes
of practice are presented here to provide guidance and
dialogue on this topic. Firstly, the American Association
of Nurse Practitioners’ (AANP) Scope of Practice for
Nurse Practitioners states that:
Nurse Practitioners assess, diagnose, treat and manage
acute episodic and chronic illnesses. They order, con-
duct, supervise and interpret diagnostic and laboratory
tests, prescribe pharmacological agents and non-
pharmacologic therapies as well as teach and counsel
patients. NPs are experts in health promotion and dis-
ease prevention. As licensed clinicians, NPs practice
autonomously and in coordination with other health care
professionals. They may serve as healthcare research-
ers, interdisciplinary consultants and patient advocates,
in addition to providing a wide range of health care ser-
vices to individuals, families, groups and communities.
(AANP, 2015)
The AANP scope of practice position paper also stipu-
lates the educational level for the NP and notes a level
of accountability and responsibility associated with pro-
viding advanced high-quality, ethical care to the public.
The Nursing Council of New Zealand (NCNZ 2017a:1)
describes the following NP scope of practice and links
the scope to six competencies that dene the know-
ledge, skills and attitudes required of them:
Nurse practitioners have advanced education, clinical
training and the demonstrated competence and legal
authority to practice beyond the level of a registered
nurse. Nurse practitioners work autonomously and in
collaborative teams with other health professionals to
promote health, prevent disease, and improve access
and population health outcomes for a specic patient
group or community. Nurse practitioners manage epi-
sodes of care as the lead healthcare provider in part-
nership with health consumers and their families/
whanau. Nurse practitioners combine advanced nurs-
ing knowledge and skills with diagnostic reasoning and
therapeutic knowledge to provide patient-centred
healthcare services including the diagnosis and man-
agement of health consumers with common and com-
plex health conditions. They provide a wide range of
assessment and treatment interventions, ordering and
interpreting diagnostic and laboratory tests, prescribing
medicines within their area of competence, and
admitting and discharging from hospital and other
healthcare service/settings. As clinical leaders, they
work across healthcare settings and inuence health
service delivery and the wider profession. Nurse
Practitioner Competencies are presented next:
1. Demonstrates safe and accountable Nurse
Practitioner practice incorporating strategies
to maintain currency and competence.
2. Conducts comprehensive assessments
and applies diagnostics reasoning to identify
health needs/problems and diagnoses.
3. Develops, plans, implements and evaluates
therapeutic interventions when managing
episodes of care.
4. Consistently involves the health consumer
to enable their full partnership in decision making
and active participation in care.
5. Works collaboratively to optimise health outcomes
for health consumers/population groups.
6. Initiates and participates in activities that support
safe care, community partnership and population
improvements.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
20
In the Republic of Ireland, Registered Advanced Nurse
Practitioners (RANP) also work within an agreed scope
of practice and meet established criteria set by the
Nursing and Midwifery Board of Ireland (NMBI 2017).
Autonomy for the NP has been highlighted within the
scope of practice by designating that the Advanced
Nurse Practitioner (ANP):
…is accountable and responsible for advanced levels of
decision-making which occur through management of
specic patient/client caseload. ANPs may conduct com-
prehensive health assessment and demonstrate expert
skill in the clinical diagnosis and treatment of acute and/
or chronic illness from within a collaboratively agreed
scope of practice framework alongside other healthcare
professionals. The crucial factor in determining Advanced
Nursing Practice, however, is the level of decision-
making and responsibility rather than the nature or dif-
culty of the task undertaken by the practitioner. Nursing
or midwifery knowledge and experience should continu-
ously inform the ANPs/AMPs decision-making, even
though some parts of the role may overlap the medical or
other healthcare professional role.
(NCMN, 2008b, p.7)
In the Republic of Ireland, this description of autonomy
is designated for both the ANP and Advanced Midwife
Practitioner (AMP).
This section emphasises the signicance of establish-
ing a scope of practice for NPs and provides examples
to consider when developing an NP scope of practice.
Identifying a scope of practice is sensitive to country
context and the healthcare settings in which the NPs
will practice. In addition, the educational programme
and curriculum design should be in alignment with the
scope of practice and competencies expected of the
NP. This is discussed next in Section 3.5.
3.5 Nurse Practitioner Education
Nurse Practitioner education varies internationally and
is inconsistent; however, a master’s degree at a post-
graduate level is considered the minimum standard for
entry level NP practice with a designation that the pro-
gramme is specically identied for the preparation of
NPs (CNA 2008; CNA 2019; Fagerstrӧm 2009; Finnish
Nurses Association 2014; NCNZ 2017b; NMBI 2017).
In the USA, there is a trend for a doctor of nursing prac-
tice (DNP) degree as entry level for NP preparation.
The credibility and sustainability of the NP concept is
supported by the educational preparation the nurse
undertakes to fulll qualications for NP practice.
Dening the educational preparation for the NP pro-
vides a basis from which to differentiate the NP from
that of the generalist nurse. Clinical competencies and
common core elements of NP clinical practice provide
the foundation for programme and curriculum develop-
ment (Nursing and Midwifery Board of Australia 2014;
CNA 2008; NCNZ 2017b; NMBI 2017).
The focus of an educational programme must be iden-
tied as the preparation of nurses to practice at an
advanced level in clinical settings as NPs. It is essential
that NP education includes supervised clinical practice
or a clinical practicum, usually for a designated min-
imum number of clinical hours with an experienced
NP or physician. The Republic of Ireland (NMBI 2017)
recommends 500 clinical hours; in the UK, the Royal
College of Nursing (RCN 2012) stipulates a minimum
of 500 supervised (direct and indirect) clinical hours;
the requirement in New Zealand is 300 hours (NCNZ,
2017b); and the prerequisite in the USA is a minimum
of 500 supervised direct patient care clinical hours
(NONPF 2017).
In New Zealand, the NP scope of practice identies six
themes or competencies expected of the applicant for
registration as a NP in the country (refer to Section 3.4
on Nurse Practitioner Scope of Practice). These
themes are linked to an NP education programme. The
NP must complete an NCNZ-accredited master’s pro-
gramme and meet the competencies for the NP scope
of practice. The programme must be clinically focused
at an advanced level. Students may choose to complete
a postgraduate diploma (registered nurse prescribing
pathway) and then complete the master’s programme
or complete the prescribing practicum towards the end
of the master’s programme. The NZ practicum for NPs
includes completion of the minimum hours of clinical
learning, completion of a clinical practice experience
diary, two in-depth case studies and a summative
assessment with a mentor as it relates to the required
competencies for NP scope of practice (NCNZ 2017b).
Competencies for the NP were established in the USA in
1990 by the National Organization of Nurse Practitioner
Faculties (NONPF) and most recently revised in 2017
(NONPF 2017). Identication of Nurse Practitioner
core competencies content is seen as supportive of
cur riculum development. In 2002, as the Advanced
Nurse Practitioner (ANP) role evolved in the UK, the
Royal College of Nursing (RCN) identied domains and
competencies based on those developed by the USA
NONPF (RCN 2010). The identied domains included
competencies that must be met by the ANP. However,
in changing with the times, Advanced Nursing Practice
in England is looking to become part of the wider
sphere of activity of Advanced Clinical Practice (ACP)
which includes a range of non-medical healthcare pro-
fessionals (HEE, 2017). The other countries of the UK
(Northern Ireland, Scotland and Wales) look to develop
their own versions of the ACP category.

20
CHAPTER THREE: THE NURSE PRACTITIONER
21
All-purpose or nonspecic master’s degree nursing
programmes are not a recommended pathway for
NPs. Master’s degree education related to nursing
management, nursing research or nursing education
alone is not considered sufcient preparation for NPs.
However, as the role evolves, existing master’s level
programmes may be adapted to include additional skills
specic to NP practice including advanced physical
assessment, advanced clinical reasoning and diagnos-
tic decision-making, pharmacology/pharmacokinetics,
clinical and professional leadership, and practice-based
research (NCNZ 2009; NMBI 2015a; NMBI 2017).
3.6 Establishing a Professional Standard for the Nurse Practitioner
Professional standards and competencies are at the
heart of a credentialing system as they dene the qual-
ity of performance required of a credentialed entity/
institution or the credentialee. Standards set the level
of education and performance for entry into practice
for the NP along with required renewal of credentials.
Competencies dene the level and quality of perform-
ance the NP is expected to demonstrate as a practicing
clinician. A dened scope of practice, a professional
standard, policies and procedures are linked with
one being the foundation for another (Jhpiego 2016).
In countries or regions without a legal or published
scope of practice for the NP, practice guidelines and
the professional standard are based on the best t for
the circumstances dictated by country context and gov-
erning processes for healthcare services. However, it is
considered optimal to establish policies, a professional
standard and regulatory mechanisms that include title
protection, a dened scope of practice and/or a job
description.
Credentialing and Regulation
for the Nurse Practitioner
Credentialing is a central function of a regulatory sys-
tem. A credential represents a level of quality and
achievement that can be expected in terms of standards
met or competence shown by the NP, the programme
of study or the institution. Regulatory mechanisms
differ and are usually linked to a country’s regulatory
traditions and resources, as well as the decision of what
level of regulation is required to recognise a nurse to
work beyond the legally recognised scope of practice
for a generalist nurse. Key in establishing a credential-
ing process for the NP is that the body providing the
credential is nationally recognised and accountable
for the methods of designated credentialing. In some
countries, credentials are renewed periodically but the
mechanisms and requirements for renewal must be
clear and transparent.
Title protection for the NP should be considered a
requirement of the regulatory and credentialing pro-
cesses. The NP title must convey a simple message of
who the NP is and should distinguish the NP from other
nursing categories and levels of nursing practice. Title
protection also safeguards the public from unqualied
clinicians who have neither the education nor the com-
petencies implied by the title.
Continuing recognition for an NP to practice commonly
requires renewal of the generalist nursing licence and
maintaining national credentialing consistent with des-
ignated professional regulation for the setting/state or
province in which the NP practices. Prescriptive authority
is a component central to full practice potential for the NP
and is governed by country, state, or provincial regulation.
Refer to Appendix 1 for Credentialing Terminology.
3.7 Nurse Practitioner Contributions to Healthcare Services
Evidence demonstrates that patients receiving care from
NPs have high satisfaction with service provision, fewer
unnecessary emergency room visits, decreased waiting
times, reduced hospital admissions and readmissions
(Begley et al, 2010; Chavez et al. 2018; Donald et al.
2015; Maier et al. 2017; Martin-Misener et al. 2015;
Newhouse et al. 2011). Studies to evaluate the quality of
care provided by NPs have shown same healthcare ser-
vices to be comparable to that of physicians in terms of
effectiveness and safety (Lentz et al. 2004; Mundinger
et al. 2000; Swan et al. 2015). A comprehensive system-
atic literature review from 2006 to 2016 in emergency
and critical care settings ndings demonstrated that
nurses in advanced practice, including NPs, reduced
length of stay, time to consultation and treatment, mor-
tality, improved patient satisfaction and cost savings
(Jennings et al. 2015; Woo et al. 2017).
The scarcity of economic evaluations of CNS and NP
roles suggests that there is limited accurate evidence
to determine their cost-effectiveness (Marshall et al.
2015). However, systematic reviews of research exam-
ining provision of healthcare services indicates that
well dened APN roles can result in reduced health-
care costs.
Refer to Appendix 3, p. 35 for country exemplars of the
Nurse Practitioner.
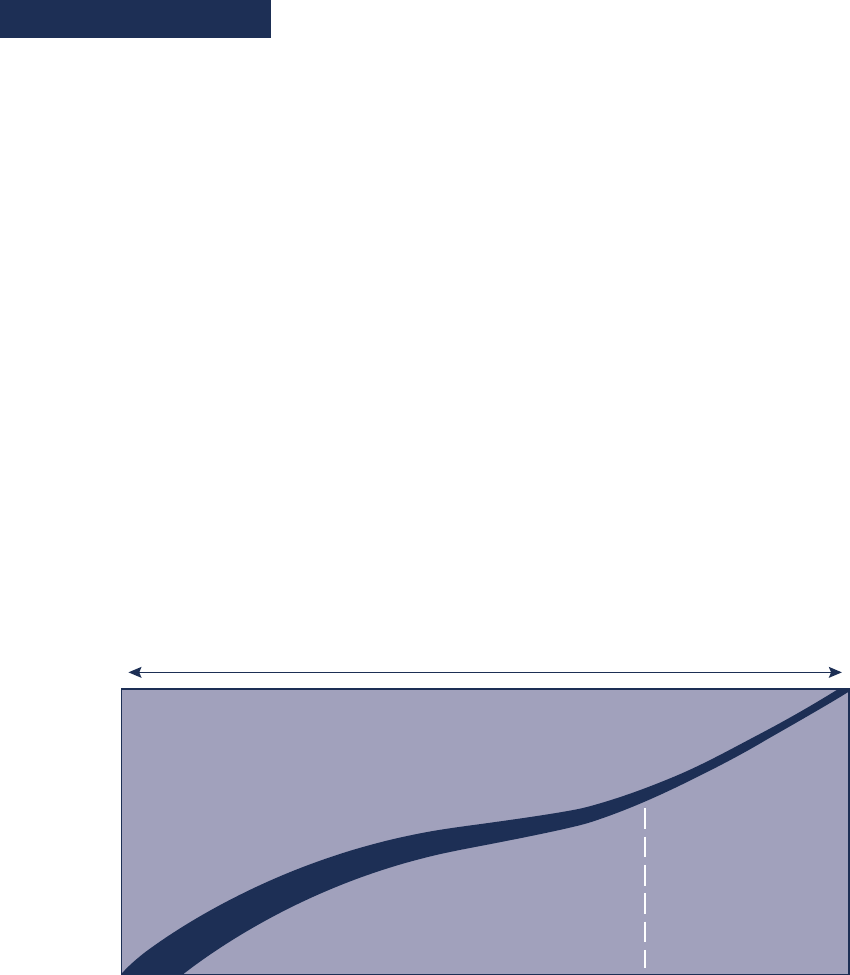
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
22
CHAPTER FOUR
DISTINGUISHING THE CLINICAL
NURSE SPECIALIST AND THE NURSE
PRACTITIONER
The origins of Advanced Practice Nursing as discussed in Chapters 2 and 3 provide historical backgrounds for the
CNS and NP, noting differences in stages of early development. The emergence of Advanced Practice Nursing
worldwide and the introduction of the concepts of the CNS and APN have resulted in robust discussions attempting
to identify the distinguishing characteristics of these new roles and levels of nursing practice. Since the mid-1990s
(Dunn 1997) and with more recent and parallel development internationally, the denitive characteristics of the
CNS and NP have become blurred. Despite this, the two roles remain largely distinct, albeit with some overlap
(Rushforth 2015; Tracy & Sendelbach 2019). This section endeavours to distinguish and clarify traits representative
of the CNS and NP.
The CNS is an expert clinician with a specialised area of practice identied in terms of population, setting, disease
or medical subspecialty, type of care or problem that includes a systems perspective to provision of healthcare
services (NACNS 2018). The focus of NP practice emphasises a population focus mainly in PHC but that now
includes both acute care and PHC (AACN Certication Corporation 2011). Bryant-Lukosius (2004 & 2008) claried
the essential distinctions between the CNS and the NP through an Advanced Practice Nursing continuum model,
emphasising how the CNS focuses more on indirect care supporting clinical excellence from a systems approach
while the NP focuses more on direct patient care within diverse clinical settings.
Figure 2: Distinction between Clinical Nurse Specialist and Nurse Practitioner
Source: Bryant-Lukosius, D. (2004 & 2008). The continuum of Advanced Practice Nursing roles. Unpublished
document.
Continuum of APN RolesCNS NP
Advanced
Nursing
Practice
Integrated Role Domains
• Professional development
• Organizational leadership
• Research
• Education
• Extended clinical
functions requiring
extended class
(EC) registration
Clinical Practice Role
A recent national study comparing CNSs and NPs in
Canada lends support to the above illustration (Bryant-
Lukosius et al. 2018). Results from this study demon-
strated that while there are many common features, the
main differences between the CNS and NP is related to
greater CNS involvement in non-clinical (indirect) activ-
ities related to support of systems, education, publica-
tion, professional leadership and research. Involvement
in direct clinical care was high for both the CNS and NP,
but differences in scope of practice were reected in
greater NP involvement in diagnosing, prescribing and
treating various conditions or illness. Similar to these
ndings, additional studies (Donald et al. 2010; Carryer
et al. 2018) highlight that NPs engage in direct care
activities to a greater extent than CNSs.

22
CHAPTER FOUR: DISTINGUISHING THE CLINICAL NURSE SPECIALIST AND THE NURSE PRACTITIONER
23
4.1 ICN Position on the Clarication of Advanced Nursing Designations
Increasingly, countries are undergoing healthcare
reform with system changes that include introducing
advanced roles and advanced levels of practice for
nurses. These dynamic changes in the perception of
how nurses provide care require the interface between
what is identied as ‘traditional’ nursing and the med-
ical profession. In addition, this transformation requires
suitable education, policy and regulation supportive of
APNs (CNSs and NPs) to practice to the full potential
of their education. Although enthusiasm for APNs such
as the CNS and NP has increased, the available data
to accurately depict APN initiatives still remains limited
thus hampering full recognition of APN presence world-
wide. Data that is available demonstrates wide vari-
ation in numbers of APNs and their practice settings
with literature mainly dominated by English language
publications originating from economically developed
countries.
It is the intent of this guidance paper to promote con-
tinued dialogue of the concept of Advanced Practice
Nursing while also seeking consistency in how APNs
are identied and integrated into healthcare systems
internationally. Not only do educational programmes
need to be specic to the designated APN (e.g. CNS
or NP) but relevant policies and a professional stand-
ard are required to promote the inclusion of sustainable
advanced nursing roles into routine healthcare service
provision.
To support future potential for the CNS and NP, there is
a need to continue to:
•
promote clarity of CNS and NP practice
•
identify how these nurses contribute to the delivery
of healthcare services
•
guide the development of educational curricula
specic to the CNS and NP
•
support these nurses in establishing advanced
practice (CNS or NP) roles and levels of practice
•
offer guidance to employers, organisations and
healthcare systems implementing the CNS and NP
•
promote appropriate governance in terms of policy,
legislation and credentialing
In an effort to offer clarity for these two categories of
nursing, ICN offers Tables 3, 4 and 5 to identify simi-
larities and distinguishing characteristics of the CNS
and NP.
Carolyn Jones
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
24
Table 3: Characteristics of Clinical Nurse Specialists and Nurse Practitioners
CLINICAL NURSE SPECIALISTS NURSE PRACTITIONERS
Dened scope of practice in an identied specialty Comprehensive scope of practice specic to the NP
with activities that include prescribing, diagnosis
& treatment management
Provides direct and indirect care usually to patients
with an established diagnosis
Commonly provides direct clinical care to patients
with un-diagnosed conditions in addition to
providing ongoing care for those with an already
established diagnosis
Works within a specialist eld of practice Works generically within a variety of elds
of practice and settings
Works in dened practice populations
(e.g. oncology, pain management, cardiology)
Works with multiple diverse practice populations
Works autonomously and collaboratively in a team,
using a systems approach, with nursing personnel
or other healthcare providers and healthcare
organisations
Works autonomously and in collaboration with other
healthcare professionals
Frequent shared clinical responsibility with other
health care professionals
Assumes full clinical responsibility and management
of their patient population
Works as a consultant to nurses and other health
care professionals in managing complex patient
care problems
Conducts comprehensive advanced health
assessments and investigations in order to make
differential diagnoses
Provides clinical care related to an established
differentiated diagnosis
Initiates and evaluates a treatment management
plan following an advanced health assessment
and investigation based on conduct of differential
diagnoses
Inuences specialist clinical and nursing practice
through leadership, education and research
Engages in clinical leadership, education
and research
Provides evidence-based care and supports nurses
and other healthcare professionals to provide
evidence-based care
Provides evidence-based care
Evaluates patient outcomes to identify
and inuence system clinical improvements
Frequently has the authority to refer and admit
patients
May or may not have some level of prescribing
authority in a specialty
Commonly has prescribing authority

24
CHAPTER FOUR: DISTINGUISHING THE CLINICAL NURSE SPECIALIST AND THE NURSE PRACTITIONER
25
Table 4: Similarities between Clinical Nurse Specialists and Nurse Practitioners
CNSs and NPs
• Have a master’s degree as a minimum educational qualication
• Are autonomous and accountable at an advanced level
• Provide safe and competent patient care through a designated role or level of nursing
• Have a generalised nursing qualication as their foundation
• Have roles with increased levels of competency that is measurable
• Have acquired the ability to apply the theoretical and clinical skills of Advanced Practice Nursing utilising
research, education, leadership and diagnostic clinical skills
• Have dened competencies and standards which are periodically reviewed for maintaining currency
in practice
• Are inuenced by the global, social, political, economic and technological milieu
• Recognise their limitations and maintain clinical competencies through continued professional
development
• Adhere to the ethical standards of nursing
• Provide holistic care
• Are recognised through a system of credentialing
Carolyn Jones
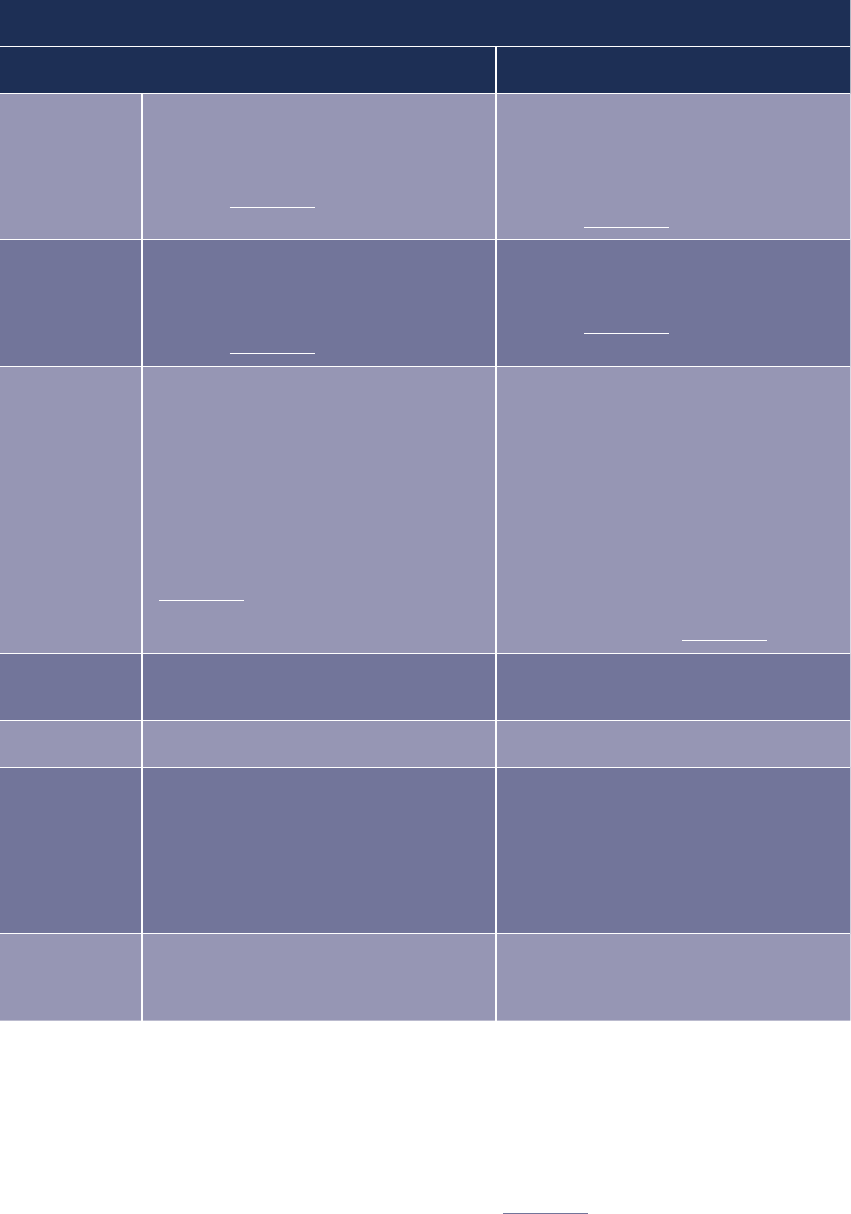

26
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
26
Table 5: Differentiating the Clinical Nurse Specialist and the Nurse Practitioner
ADVANCED PRACTICE NURSING
Clinical Nurse Specialist Nurse Practitioner
Education Minimum standard master’s degree
Accredited programme specic to the CNS
Identied specialty explicit to CNS practice
(Refer to Section 2.5)
Minimum standard master’s degree
Accredited programme specic to the NP
Generalist-commonly PHC or
acute care explicit to NP practice
(Refer to Section 3.5)
Denition Expert advanced practice clinicians
providing direct complex specialty
care along with a systems approach
to the provision of healthcare services
(Refer to Section 2.3)
Autonomous clinicians who are able
to diagnose and treat conditions based
on evidence-informed guidelines
(Refer to Section 3.3)
Scope of
Practice
Job
Description
Specialty practice aimed to ensure and
develop the quality of nursing, foster
the implementation of evidence- based
nursing and support the hospital or
organisation’s strategic plan for provision
of healthcare services by providing direct
and indirect healthcare services. The
CNS provides leadership in advancing
nursing practice including research and
interdisciplinary education (Refer to
Section 2.3)
Comprehensive healthcare practice,
autonomous examination and assessment
of patients that includes initiating
treatment and developing a management
plan. Management commonly includes
authority to prescribe medications and
therapeutics, and conducting referrals
along with monitoring acute and chronic
health issues, primarily in direct healthcare
services. Practice includes integration
of education, research and leadership in
conjunction with the emphasis on direct
clinical care. (Refer to Section 3.4)
Work
settings
Commonly based in hospital or healthcare
institutional settings with a specialty focus
Commonly based in PHC and other out
of hospital settings or acute care
Regulation Legally protected title Legally protected title
Credentialing Licensure, certication or authorisation
by a national governmental or
nongovernmental agency specic
to practice as a CNS. Submission
of evidence of completion of a CNS
programme from an accredited school
of nursing
Licensure, certication or authorisation
by a national governmental
or nongovernmental agency specic
to practice as an NP. Submission
of evidence of completion
of an NP programme from an accredited
school of nursing
Policy An explicit professional standard including
specic criteria and policies to support
the full practice potential of the CNS
An explicit professional standard including
specic criteria and policies to support
the full practice potential of the NP
In taking this position, ICN recognises the continued
need to present guidance for discussion in order to
meet the changing healthcare demands of diverse
populations and associated healthcare systems along
with the changing dimensions of nursing practice. This
guidance paper summarises the current situation inter-
nationally in respect to the CNS and NP and provides
a foundation for moving forward. Advanced Practice
Nursing will continue to progress in its development
and these professionals should have formal education
that responds to the highest standards of the role or
level of nursing. Topics that warrant further in-depth dis-
cussion include issues of governance, education and
ongoing research within and between countries, along
with exploration of Advanced Practice Nursing beyond
that of the CNS and NP.
Refer to Appendix 4 for exemplars where countries use
a combination of the concepts of CNS and NP. In sev-
eral cases the title used is Advanced Practice Nurse
when combining attributes of the CNS and NP.

REFERENCES
26 2726
REFERENCES
American Association of Colleges of Nursing (AACN) (undated). AACN Statement of Support for Clinical Nurse
Specialists.
American Association of Colleges of Nursing (AACN) Certication Corporation (2011). ppt accessed 24 October 2018
from www.aacn.org media website.
American Association of Nurse Practitioners (AANP) (2015). Scope of Practice for Nurse Practitioners. Position
Paper.
American Association of Nurse Practitioners (AANP) (2018). What’s an NP? Accessed September 5, 2018 from
www.aanp.org/all-about-nps/what-is-an-np.
American Nurses Association (2004). Nursing: Scope & Standards of Practice. Washington, DC: American Nurses
Association.
American Nurses Association (2015). Nursing: Scope and Standards of Practice, 3
rd
. Ed. Silver Spring, MD; ANA.
ISBN: 978-1-55810-619-2; PUB# 9781558106192.
APRN Consensus Group Work Group & NCSBN APRN Advisory Committee. (2008). Consensus Model for APRN
regulation: Licensure, Accreditation, Certication, and Education. Available at: http://www.nonpf.org/associa-
tions/10789/les/APRNConsensusModelFinal09.pdf.
Barton TD, Allan D (2015). Advanced Practice: Changing Healthcare in a Changing World. London: Palgrave/
Macmillan Publishers Limited.
Barton D, East L (2015). The Evolution of Advanced Nursing Practice. In T.D. Barton, D. Allan (Eds.) Advanced
Nursing Healthcare in a Changing World. London: Palgrave/Macmillan Publishers Limited. pp. 1 – 19.
Begley C, Murphy K, Higgins A, Elliott N, Lalor J, Sheerin F, Coyne I, Comiskey C, Normand C, Casey C, Dowling M,
Devane D, Cooney A, Farrelly F, Brennan M, Meskell P, MacNeela P (2010). Evaluation of Clinical Nurse and
Midwife Specialist and Advanced Nurse and Midwife Practitioner Roles in Ireland (SCAPE) Final Report. National
Council for the Professional Development of Nursing and Midwifery in Ireland, Dublin.
Brown-Brumeld D, DeLeon A (2010). Adherence to a medication safety protocol: Current practice for labeling
medications and solutions on the sterile eld. Association of Operating Room Nurses Journal, 91, pp. 610 – 617.
Bryant-Lukosius D (2004 & 2008). The Continuum of Advanced Practice Nursing Roles. Unpublished document.
Bryant-Lukosius D, Carter N, Kilpatrick K, Martin-Misener R, Donald F, Kaasalainen S, DiCenso A (2010). The Clinical
Nurse Specialist in Canada. Nursing Leadership, 23 (Special Issue), 140-166. doi:10.12927/cjnl.2010.22273.
Bryant-Lukosius D, Callens D, De Geest S, Degen Kellerhals S, Fliedner M, Grossman F, Henry M, Herrmann L,
Koller A, Martin J, Schwendimann R, Spichiger E, Stoll H, Ulrich A, Wreibel L (2015). Advanced Nursing Practice
Roles in Switzerland: A Proposed Framework for Evaluation. Basel, Switzerland: Institute of Nursing Science,
University of Basel.
Bryant-Lukosius D, Carter N, Reid K, Donald F, Martin-Misener R, Kilpatrick K, Harbman P, DiCenso A (2015).
The clinical effectiveness and cost-effectiveness of Clinical Nurse Specialist-led hospital to home transitional care:
A systematic review. Journal of Evaluation of Clinical Practice, 21, pp. 763-781.
Bryant-Lukosius D, Cosby R, Bakker D, Earle C, Burkoski V (2015). Practice Guideline on the Effective Use of
Advanced Practice Nurses in the Delivery of Adult Cancer Services in Ontario. Toronto: Cancer Care Ontario.
Available at: https://www.cancercareontario.ca/en/guidelines-advice/types-of-cancer/2166.
Bryant-Lukosius D, Martin-Misener R (2016). ICN Policy Brief Advanced Practice Nursing: An Essential Component
of Country Level Human Resources for Health. Geneva.
Bryant-Lukosius D, Valaitis R, Martin-Misener R, Donald F, Moran Pena L, Brosseau L (2017). Advanced Practice
Nursing: A strategy for achieving universal health coverage and universal access to health. Revista Latino-
americano de Enfermagem, 25, e2826, doi: 10.1590/1518-8345.1677.2826.
Bryant-Lukosius D, Jokiniemi K, Martin-Misener R, Roussel J, Carr M, Kilpatrick K, Tramner J, Y Rietloetter S
(2018). Clarifying the contributions of specialized nursing roles in Canada: Results of a national study. Panel pres-
entation. Canadian Nurses Association Conference, Ottawa, ON. June 20.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
28
Bryant-Lukosius D, Wong FKY (2019). International Development of Advanced Practice Nursing. In M.F. Tracy
& E.T. O’Grady (eds). Advanced Practice Nursing: An Integrative Approach, 6
th
edition, pp. 129-141, St. Louis,
Missouri: Elsevier.
Canadian Nurses Association (CNA) (2008). Advanced Nursing Practice: A National Framework. Ottawa: Author.
Canadian Nurses Association (CNA) (2014). Core Competencies for the Clinical Nurse Specialist in Canada.
Ottawa: Author.
Canadian Nurses Association (CNA) (2016a). The Canadian Nurse Practitioner Initiative: A 10 year Retrospective.
Ottawa: Author.
Canadian Nurses Association (CNA) (2016b). Position Statement Clinical Nurse Specialist. Ottawa: Author.
Canadian Nurses Association (CNA) (2018) Nurse Practitioners. Retrieved 8 September 2018 from: https://cna-
aiic.ca/en/professional-development/advanced-nursing-practice/nurse-practitioners.
Canadian Nurses Association (CNA) (2019) Advanced Practice Nursing: A Pan-Canadian Framework. Author:
CNA, Ottawa, Canada.
Cary AH, Smolenski MC (2018). Credentialing and Clinical Privileges for the Advanced Nurse. In L. Joel (Ed.)
Advanced Practice Nursing: Essentials for Role Development. 4
th
Edition. pp. 100 – 115, Philadelphia: F.A. Davis.
Carryer J, Wilkinson J, Towers A, Gardner G (2018). Delineating Advanced Practice Nursing in New Zealand:
A national survey. International Nursing Review, 65(1) pp. 24 – 32.
Cassiani SHDB, Zug KE (2014). Promoting the Advanced Nursing Practice role in Latin America. Revista Brasileira
de Enfermagen. 67(5) pp. 673-674. doi: 10.1590/0034-7167.2014670501.
Chan GK, Cartwright CC (2014). The Clinical Nurse Specialist. In A.B. Hamric, C.M. Hanson, M.F. Tracy, E.T.
O’Grady (Eds.) Advanced Practice Nursing: An Integrative Approach. 5
th
Edition. St. Louis: Elsevier Saunders.
pp. 359 – 395.
Chavez K, Dwyer A, Ramelet A (2018). International practice settings, interventions and outcomes of Nurse
Practitioners in geriatric care: A scoping review. International Journal of Nursing Studies. 78, pp 61-75. doi:
10.1016/j.ijnurstu.2017.09.010. Epub 2017 Sep 18.
Cockerham AZ, Keeling AW (2014). A Brief History of Advanced Practice Nursing in the United States. In A.B. Hamric,
C.M. Hanson, M.F. Tracy, E.T. O’Grady (Eds.) Advanced Practice Nursing: An Integrative Approach. 5
th
Edition.
St. Louis: Elsevier Saunders. pp. 1 – 26.
Cook O, McIntyre M, Recoche K (2015). Exploration of the role of specialist nurses in the care of women with
gynaecological cancer: A systematic review. Journal of Clinical Nursing, 24(5-6), pp. 683-695.
Cooper MA, Docherty E (2018). Transforming the landscape. Comment. British Journal of Nursing, 27(21) p. 1216.
Delamaire M, Lafortune G (2010) Nurses in advanced roles: A description and evaluation of experiences in 12 devel-
oped countries. OECD Working Health Working Papers No. 54, OECD Publishing. doi.org/10.1787/5kmbrcfms5g7-en.
Donald F, Bryant-Lukosius D, Martin-Misener R, Kassalainen S, Kilpatrick K, Carter N, Harbman P, Bourgeault
I, DiCenso A (2010). Clinical Nurse Specialists and Nurse Practitioners: Title confusion and lack of role clarity,
Nursing Leadership 23 (Special Issue) pp. 189 – 210. doi: 10.12927/cjnl.2010.22276.
Donald F, Kilpatrick K, Reid K, Carter N, Martin-Misener R, Bryant-Lukosius D, Kassalainen S, Marshall DA,
Charbonneau-Smith R, Donald EE, Lloyd M, Wickson-Grifths A, Yost J, Baxter P, Sangster-Gormley E, Hubley P,
Laamme C, Campbell-Yeo M, Price S, Boyko J, DiCenso A (2014). A systematic review of the cost-effectiveness
of Nurse Practitioners and Clinical Nurse Specialists: What is the quality of the evidence? Nursing Research and
Practice. doi: 10.1155/2014896587.
Donald F, Kilpatrick K, Carter N, Bryant-Lukosius D, Martin-Misener R, Kassalainen S, Harbman P, Marshall D,
Reid K, DiCenso A (2015). Hospital to community transitional care by Nurse Practitioners. A systematic review of
cost-effectiveness. International Journal of Nursing Studies. Jan;52(1):436-451. doi:10.1016/j.ijnurstu.2014.07.011.
Dunn L (1997). A literature review of advanced clinical nursing practice in the United States. Journal of Advanced
Nursing 25: pp. 814-819.
Dunphy LM, Flinter MM, Simmonds KE (2019). The primary care Nurse Practitioner. In M. F. Tracy, E.T. O’Grady
(eds), Advanced Practice Nursing: An integrative approach, 6
th
Edition, St. Louis, Missouri: Elsevier Inc.

REFERENCES
28 29
European Specialist Nurses Organizations (ESNO) (2015). Competences of the Clinical Nurse Specialist (CNS):
Common plinth of competences for the common training framework of each specialty. Version 1, 17-10-2015.
Fagerström L (2009). Developing the scope of practice and education for Advanced Practice Nurses in Finland.
International Nursing Review, 56, pp 269‐272.
Flanders S, Clark AP (2010). Interruptions and medication errors. Clinical Nurse Specialist, 24, pp. 281 – 285.
Finnish Nurses Association (2016). New roles for nurses – quality to future social welfare and health care services.
English translation accessed September 8, 2018. Available at: https://sairaahoitajat./wp-content/uploads/2018/06/
apn_raportti_eng_valmis_pieni.pdf.
Fulton J, Holly V (2018). Characteristics of the CNS role and practice. Personal communication April 2018.
Gardner G, Chang AM, Dufeld C, Doubrovsky A (2013). Delineating the practice prole of Advanced Practice
Nursing: a cross-sectional survey using the modied Strong Model of advanced practice. Journal of Advanced
Nursing, 69(9) pp. 1931-1942.
Gardner G, Dufeld C, Doubrovsky A & Adams M (2016). Identifying advanced practice: A national survey of a
nursing workforce. International journal of nursing studies, 55, pp. 60-70.
Gardner G, Dufeld C & Gardner A (2017). The Australian Advanced Practice Nursing Self-Appraisal Tool (The
ADVANCE Tool). Queensland University of Technology.
Gardner G, Dufeld C, Doubrovsky A, Adams M (2015). Identifying advanced practice: a national survey of a nurs-
ing workforce. International Journal of Nursing Studies, 55 pp. 60-70.
Government of Ireland (1998). Report of the Commission on Nursing. A Blueprint for the Future. Available at:
https://health.gov.ie/wp-content/uploads/2014/03/Report-of-The-Commision-on-Nursing.pdf.
Hamric AB, Tracy MF (2019). A denition of Advanced Practice Nursing. In M.F. Tracy & E.T. O’Grady (eds)
Advanced Practice Nursing: An integrative approach, 6
th
Edition, St. Louis: Elsevier, pp. 61 – 79.
Hannon RA, Ray SL & Staples E (2016). Canadian perspectives on Advanced Practice Nursing. Toronto: Canadian
Scholars Press.
Hanson, C.M. Hamric A.B. Reections on the continuing evolution of Advanced Practice Nursing. Nursing Outlook,
2003. 51(5): pp. 203-211.
Health Education England (HEE) (2017). Multi-professional Framework for Advanced Clinical Practice https://www.
hee.nhs.uk/sites/default/les/documents/Multi-professional%20framework%20for%20advanced%20clinical%20
practice%20in%20England.pdf.
Hill MN, Parker J, Liu H, Hu Y, Guo G (2017). Strategic directions and actions for Advanced Practice Nursing in
China. International Journal of Nursing Sciences, 4(1), pp. 8-11.
Horrocks S, Anderson A, Salisbury C (2002). Systematic review of whether Nurse Practitioners working in pri-
mary care can provide equivalent care to doctors. British Medical Journal, 324, 819. doi: https://doi.org/10.1136/
bmj.324.7341.819.
International Council of Nurses (ICN) (2008a). The scope of practice, standards and competencies of the Advanced
Practice Nurse. Monograph, ICN Regulation Series. Author: Geneva.
International Council of Nurses (ICN) (2008b). Nursing care continuum framework and competencies. Monograph,
ICN Regulation Series. Author: Geneva.
Irinoye OO (2011). North-South collaboration for the advancement of nursing education and quality health care in
Nigeria – Report on proposal for collaboration between University of Maryland School of Nursing, Ofce of Global
Health, Baltimore and Department of Nursing Science, Obafemi Awolowo University, ILE-IFE (unpublished paper).
Jennings N, Clifford S, Fox AR, O’Connell J, Gardner G (2015). The impact of Nurse Practitioner services on cost,
quality of care, satisfaction and waiting times in the emergency department: a systematic review. International
Journal of Nursing Studies, 52(1):421-35. doi: 10.1016/j.ijnurstu.2014.07.006.
Jhpiego (2016). Scope, standards, policies and procedures model. Accessed September 7, 2018 from https://
reprolineplus.org/system/les/resources/o3_SSPP%20Model_tc.pdf.
Kaasalainen S, Martin-Misener R, Kilpatrick K, Harbman P, Bryant-Lukosius D, Donald F, Carter N & DiCenso A
(2010). Historical overview of Advanced Practice Nursing roles in Canada. Canadian Journal of Nursing Leadership,
23, 35- 60.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
30
Keeling AW, Bigbee JL (2005). The history of advanced practice in the United States. In A.B. Hamric, J.A. Spross,
C.M. Hanson (Eds.) Advanced Practice Nursing: an integrative approach. 3
rd
Edition. St. Louis: Elsevier Saunders.
pp. 3 – 45.
Kilpatrick K, DiCenso A, Bryant-Lukosius D, Ritchie JA, Martin-Misener R, Carter N (2013). Practice patterns and
perceived impact of Clinical Nurse Specialist roles in Canada: Results of a national survey. International Journal
of Nursing Studies, 50(110), 1524-1536.
Kilpatrick K, Kaasalainen S, Donald F, Reid K, Carter N, Bryant-Lukosius D, Martin-Misener R, DiCenso A (2014).
The effectiveness and cost-effectiveness of Clinical Nurse Specialists in outpatient roles: A systematic review.
Journal of Evaluation in Clinical Practice. July 5, doi: 10.1111/jep.12219.
Kim MY (2011). Effects of oncology Clinical Nurse Specialists’ interventions on nursing-sensitive outcomes
in South Korea. Clinical Journal of Oncology Nursing, 15. E66-74. doi: 10.1188/11.ONF.E66-E74.
Leary A, Crouch H, Lezard A, Rawcliffe C, Boden, L, Richardson A (2008). Dimensions of Clinical Nurse Specialist
work in the UK. Nursing Standard (Royal College of Nursing), 23(15) 40-44. doi:10.7748/ns2008.12.23.15.40.c6737.
Lentz ER, Mundinger MO, Kane RL, Hopkins SC, Lin SX (2004). Primary care outcomes by Nurse Practitioners
in patients treated by Nurse Practitioners or physicians: Two year follow-up. Medical Care Research and Review,
61(3) pp. 332-351.
Lewandowski WS, Adamle K (2009). Substantive areas of Clinical Nurse Specialist practice: A comprehensive
review of the literature. Clinical Nurse Specialist, 23, pp. 73-90.
Maier C, Aiken L & Busse R (2017). Nurses in advanced roles in primary care: policy levers for implementation,
OECD Health Working Paper no. 98, OECD, Paris. doi.org/10.1787/a8756593-en.
Marshall DA, Donald F, Lacny S, Reid K, Bryant-Lukosius D, Carter N, Charbonneau-Smith R, Harbman P,
Kaasalainen S, Kilpatrick K, Martin-Misener R, DiCenso A (2015). Assessing the quality of economic evaluations
of Clinical Nurse Specialists and Nurse Practitioners: A systematic review of cost-effectiveness. NursingPlus Open,
11-17 doi: 10.1016/j.npls.2015.07.001.
Martin-Misener R, Harbman P, Donald F, Reid K, Kilpatrick K, Carter N, Bryant-Lukosius D, DiCenso A (2015). Cost-
effectiveness of Nurse Practitioners in ambulatory care: systematic review. BMJ Open 5:e007167 doi:10.1136/
bmjopen-2014-007167.
Miranda Neto MV, Rewa T, Leonello VM, Oliveira MAC (2018). Advanced Practice Nursing: a possibility for primary
health care? Rev Bras Enferm [internet]. 2018; 71 (Supl 7): pp. 716-721. doi: 10.1590/0034-7167-0672.
Mundinger MO, Kane RL, Lenz ER (2000). Primary care outcomes in patients treated by Nurse Practitioners or
physicians. JAMA, 283(1)59-68, doi: 10.1001/jama.283.1.59.
National Association of Clinical Nurse Specialists (NACNS) (2004). Model Rules and Regulations for CNS Title
Protection and Scope of Practice. Author: Harrisburg, PA, USA.
National Association of Clinical Nurse Specialists (NACNS) (2010). National CNS Competency Task Force:
Executive Summary, Author: Harrisburg. PA, USA.
National Association of Clinical Nurse Specialists (NACNS) (2018) What is a Clinical Nurse Specialist? Accessed
24 January 2018 from http://nacns.org/about-us/what-is-a-cns/.
National Council for the Professional Development of Nursing and Midwifery (2007). Framework for the establish-
ment of Clinical Nurse/Midwife Specialist posts: Intermediate Pathway. 3
rd
Edition. NCNM: Dublin, Ireland.
National Council for the Professional Development of Nursing and Midwifery (NCNM) (2008a). Proles of Advanced
Nurse/Midwife Practitioners and Clinical Nurse/Midwife Specialists in Ireland. Author: NCNM, Dublin, Ireland.
National Council for the Professional Development of Nursing and Midwifery (NCNM) (2008b). Framework for the
Establishment of Advanced Nurse Practitioner and Advanced Midwife Practitioner Posts 4
th
Edition. Author: NCNM,
Dublin, Ireland.
National Organization of Nurse Practitioner Faculties (NONPF) (2017). Nurse Practitioner core competencies con-
tent. Author: NONPF.
Newhouse RP, Stanik-Hutt J, White KM, Johantgen M, Bass EB, Zangaro G, Wilson RF, Fountain L, Steinwachs DM,
Heindel L, Weiner JP (2011). Advanced Practice Nurse outcomes 1990-2008: A systematic review. Nursing
Economics, 29/5, CNE Series.
REFERENCES
30 31
Northern Ireland Practice and Education Council for Nursing and Midwifery (NIPEC) (2014). Advanced Nursing
Practice framework: Supporting Advanced Nursing Practice in health and social care trusts. Department of Health,
Social Services and Public Safety (www.dhsspsni.gov.uk).
Nursing Council for the Professional Development of Nursing and Midwifery (NCNM) (2008). Framework for the
establishment of Advanced Nurse Practitioner and Advanced Midwife Practitioner posts. 4
th
Edition.
NPAC-AIIPC (2018). Nurse Practitioner denition in Canada. Accessed April 4, 2019 from https://npac-aiipc.org
Nurse Practitioner Association in Canada, Nova Scotia.
Nursing Council of New Zealand (NCNZ) (2017a). Competencies for the Nurse Practitioner scope of practitioner.
Author: NCNZ.
Nursing and Midwifery Board of Australia (NMBA) (2014). Nurse Practitioner standards of practice.
Nursing and Midwifery Board of Australia (NMBA) (2018). Nurse Practitioner standards of practice (update
March 2018).
Nursing and Midwifery Board of Ireland (NMBI) (2015a) Ionising radiation, nurse prescriptive authority. Standards
and Requirements. Author: NMBI.
Nursing and Midwifery Board of Ireland (NMBI) (2015b). Prescriptive Authority for Nurses and Midwifes. Standards
and Requirements. Author: NMBI.
Nursing and Midwifery Board of Ireland (NMBI) (2017) Advanced practice (nursing) standards and requirements.
Author: NMBI.
O’Connor T (2016). So what’s a Clinical Nurse Specialist exactly? Kai Tiaki Nursing New Zealand, 22(2) pp 15-16.
Ofce of the Chief Nurse, Department of Health (2017). Developing a Policy for Graduate, Specialist and Advanced
Nursing & Midwifery Practice Consultation Paper. Author: DoH.
Prostate Cancer UK (2014). The specialist nursing workforce caring for men with prostate cancer in the UK.
Research report 2014. Commissioned by Prostate Cancer UK.
Royal College of Nursing (RCN) (2008). Advanced Nurse Practitioners - an RCN guide to the Advanced Nurse
Practitioner role, competencies and programme accreditation. London: Author.
Royal College of Nursing (RCN) (2010). RCN competencies-Advanced Nurse Practitioners. An RCN guide to the
Advanced Nurse Practitioner role, competences and programme accreditation. Retrieved 5 October 2018 from
http://www.wales.nhs.uk/sitesplus/documents/8.
Royal College of Nursing (RCN) (2012). Advanced Nurse Practitioners: An RCN guide to Advanced Nursing
Practice, Advanced Nurse Practitioners, and programme accreditation. London: Author.
Royal College of Nursing (RCN) (2018). RCN credentialing for advanced level nursing practice: Handbook for
applicants. London: RCN Credentialing.
Rushforth H (2015). Advanced Nursing Practice: The theoretical context and evidence base. In T.D. Barton,
D. Allan (Eds.) Advanced Nursing Practice: Changing healthcare in a changing world. London: Palgrave/Macmillan
Publishers Limited. pp. 21 – 49.
Sangster-Gormley (2007) Nurse Practitioner sensitive outcomes. Halifax: College of Nurses Nova Scotia, Canada.
Schober M, Affara FA (2006). Advanced Nursing Practice. Oxford: Blackwell Publishing Ltd.
Schober M (2016). Introduction to Advanced Nursing Practice: An international focus. Cham, Switzerland: Springer
International Publishing AG.
Schober M (2017). Strategic planning for Advanced Nursing Practice. Cham, Switzerland: Springer International
Publishing AG.
Schober M, Green A (2018). Global perspectives on Advanced Nursing Practice. In L. Joel (Ed.) Advanced Practice
Nursing, 4
th
Edition, pp. 55 – 89, Philadelphia: F.A. Davis.
Schreiber R, MacDonald M, Pauly B, Davidson H, Crickmore J, Moss L, Regan S, Hammond C (2005). Singing
in different keys: Enactment of Advanced Nursing Practice in British Columbia. Canadian Journal of Nursing
Leadership Online Exclusive June: 1-17.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
32
Scottish Government (2008). Supporting the development of Advanced Nursing Practice: A toolkit approach.
Author: CNO Directorate, Scottish Government.
Seitio-Kgokgwe O, Gauld RDC, Hill PC, Barnett P (2015). Development of the national health information sys-
tems in Botswana: Pitfalls, prospects and lessons. Online Journal of Public Health Informatics. doi: 10.5210/ojphi.
v7/2.5630.
Sibanda B, Stender SC (2018). Anglophone Africa Advanced Practice Nurse Coalition Project (AAAPNC):
A Proposal to WHO (Africa) Health Systems Leadership. Unpublished document.
Steinke MK, Rogers M, Lehwaldt D, Lamarche K (2017). An examination of Advanced Practice Nurses’ job satis-
faction internationally. INR, 65(2) doi:org/10.1111/inr.12389.
Swan M, Ferguson S, Chang A, Larson E, Smaldone A (2015). Quality of primary care by Advanced Practice
Nurses: A systematic review. Int J Qual Health Care, 27(5): 396-404, doi: 10.1093/intqhc/mzv054.
Tracy MF, O’Grady ET (2019). Advanced Practice Nursing: An integrative approach, 6
th
Edition, St. Louis: Elsevier.
Tracy MF, Sendelbach S (2019). The Clinical Nurse Specialist. In M.F. Tracy & E.T. O’Grady (eds) Advanced
Practice Nursing: An integrative approach, 6
th
Edition, St. Louis: Elsevier, pp. 343 – 373.
Prostate Cancer UK (2014). The specialist nursing workforce caring for men with prostate cancer in the UK:
Research report. Author: Prostate Cancer UK.
World Health Organization-Eastern Mediterranean Region (WHO-EMRO) (2018). Regional guide for the develop-
ment of nursing specialist practice. Author: Cairo.
Wongkpratoom S, Srisuphan W, Senaratana W, Nantachaipan P, Sritanyarat W (2010). Role development of
Advanced Practice Nurses in Thailand. Pacic Rim International Journal of Nursing Research 2010, 14(2)
pp.162-177.
Woo BFY, Lee JXY, Tam WWS (2017). The impact of the Advanced Practice Nursing role on quality of care, clinical
outcomes, patient satisfaction, and cost in the emergency and critical care settings: A systematic review. Human
Resources in Health 15:63, doi: 10.1186/s12960-017-0 237-9.
Carolyn Jones
APPENDICES
32 33
APPENDICES
Appendix 1: Credentialing Terminology
ACCREDITATION A process of review and approval by a recognised agency by which an institution
or programme is granted time-limited recognition of having met established
standards.
CERTIFICATION The formal recognition of knowledge, skills and experience demonstrated by the
achievement of the professional standard set for the CNS or NP. Recognition of
competence for a CNS or NP who has met pre-established eligibility requirements
and standards.
EDUCATION The formal preparation of the CNS or NP: at a master’s degree or beyond that
of a generalist nurse.
LICENSURE The granting of the authority to practice. The process, sanctioned by law,
of granting exclusive privilege to CNSs or NPs meeting established standards,
which allows the CNS or NP to practice and to use the specically protected title
of CNS or NP.
REGISTRATION In a basic sense registration means that an individual’s name has been entered
into an ofcial register for persons who possess the specic qualications for CNS
or NP. The register is maintained by a regulatory or another ofcial governmental
body and usually provides title protection. The register is not a validation of
competence for the CNS or NP but simply a listing or registration of the position.
(Sources: Schober & Affara 2006; Cary & Smolenski 2018)
Appendix 2: The International Context and Country Examples of the CNS
At times, the contributions of the CNS are not always
visible in the healthcare sectors or programmes where
these nurses practice; literature describing the CNS
impact on care is sparse and the terms specialist and
Clinical Nurse Specialist are often used interchangeably
with varied credentials. These factors present a confus-
ing picture when attempting to present an international
CNS prole. It is beyond the scope of this paper to iden-
tify all countries where the CNS role is present, but this
appendix offers country context and exemplars where
the CNS role is established and identiable.
A general overview indicates that in Japan, the rst
CNS master of nursing graduate programme was in
psychiatric/mental health nursing and graduated its
rst students in 1986. By 2005, Japan had 139 nurses
practicing as a CNS (Schober & Affara 2006). The rst
CNS in Taiwan was employed in 1994 in cardiac sur-
gery. The Hospital Authority of Hong Kong introduced
the nurse specialist (not currently identied as a CNS)
in 1994 hoping that it would motivate nurses to remain
in clinical practice. In South Korea, the Oncology CNS
began working at one South Korean hospital in 1994.
To earn national CNS certication (established in 2005)
nurses must prepare at the master’s level of education
and pass an examination. Early evaluation of this role
provides indications of positive impact on oncology
patient care (Kim 2011). The Thai perspective for the
CNS emphasises specialisation and expansion of nurs-
ing and has been based on the American model in six
specialty areas (maternal/newborn, pediatrics, medical/
surgical, mental health/psychiatric, community health
and gerontology) (Wongkpratoom et al. 2010).
Iceland traces the development of the CNS in hospital
settings to the return of nurses from the USA with mas-
ter’s qualications (Schober. 2016). Roles similar to the
CNS have emerged in other Nordic countries in order
to promote research and develop expert clinical roles
mainly in conditions such as diabetes, hypertension and
psychiatric ailments. Switzerland is in its early develop-
ment and evaluation of the CNS role (Bryant-Lukosius
et al. 2015). Rushforth (2015) considers development
of the CNS role in the UK to be inconsistent and not
clearly dened.
The following case exemplars provide in-depth country
descriptions of successful CNS development.
Canada
CNSs were introduced in Canada to provide highly
complex and specialised care, develop nursing prac-
tice, support nurses at the point-of-care, and lead qual-
ity improvement and evidence-based practice initiatives
in response to research advances in treatment and
technology (Bryant-Lukosius & Martin-Misener 2015).
Three areas of CNS practice include management and
care of complex and vulnerable populations, education
and support of interdisciplinary staff, and facilitation of
change and innovation within the health-care system
(Lewandowski & Adamle 2009). Their clinical role within
the healthcare organisation enables them to identify
care and resource gaps to improve client ow and clin-
ical outcomes as well as to enhance health system pol-
icies (CNA 2019).

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
34
The CNS in Canada does not have a protected title
and standardised educational programmes are not yet
available (Bryant-Lukosius et al. 2010; CNA 2012; CNA
2019). Canadian researchers (Bryant-Lukosius et al.
2018) found that lack of regulation and title protection
poses barriers to CNS full practice potential. This situ-
ation for CNSs in Canada appears to be related to the
mix of master’s- and non-master’s-educated Advanced
Practice Nurses working as specialists without clear
avenues for career advancement, education, cre-
dentialing, or methods for knowing which nurses are
practicing safely at an advanced level. As a result, the
public, health care providers, and administrators are
uncertain about what CNSs have to offer and may have
unclear expectations about the CNS scope of practice.
This lack of clarity and uncertainty poses a risk for the
recruitment and retention of CNSs despite evidence
supporting the positive impact of the role in the country
(CNA, 2019).
New Zealand
In New Zealand, the CNS role has no formal or legal
denition thus there is confusion about the CNS and
the relevant scope of practice (O’Connor 2016). The
qualications required for a CNS to practice in New
Zealand vary at the discretion of employers. A study
conducted in New Zealand, that replicated a study con-
ducted in Australia, noted that the scope of practice for
the NP and CNS may overlap but are not interchange-
able (Carryer et al. 2018). Study ndings indicate that
the CNS position in New Zealand equates to the clin-
ical nurse consultant in Australia and, similar to studies
conducted in Australia (Gardner et al. 2013 & 2015),
are the only roles to be dened as Advanced Practice
Nursing roles. Carryer et al (2018) suggest that the
more prevalent presence of the CNS in New Zealand
may be related to employment practices that favor CNS
appointments that in turn translate to opportunities for
this type of APN practice.
Republic of Ireland
The framework for the development of the CNS in
Ireland provides the requirements for nurses seeking
this position. The CNS is viewed as a dened advanced
area of nursing practice that requires application of spe-
cially focused knowledge and skills, which are both in
demand and required to improve the quality of patient/
client care in the country. (National Council for the
Professional Development of Nursing and Midwifery
2007).
The practice of a CNS includes a focus which consists
of assessment, planning, coordination and provision
of care, health promotion and patient education. They
also communicate and negotiate decisions in collab-
oration with other healthcare professionals and commu-
nity resource providers. CNSs represent patient/client
values in hospital, community and outpatient settings.
The CNS works closely with medical and para- medical
colleagues and may make alterations in prescribed
clinical options along agreed protocol driven guide-
lines. Specic responsibilities are represented in a job
description rather than the position title.
CNS practice in Ireland is divided into direct and indi-
rect care (see Section 2.2 in this paper). Similar to
other country exemplars, direct care comprises the
assessment, planning, coordination, delivery and
evaluation of care and education to patients and their
families. Indirect care relates to activities that inuence
others in their provision of direct care. In this capacity,
the CNS participates in and implements nursing/clinical
research, audits and provides consultancy in educa-
tion and clinical practice to nursing colleagues and the
wider interdisciplinary team. CNSs are, in tandem with
their line manager, responsible for their continuing pro-
fessional development, including participation in formal
and informal educational activities, thereby ensuring
sustained clinical credibility among nursing, medical
and paramedical colleagues (National Council for the
Professional Development of Nursing and Midwifery,
2007).
Japan
The Japanese Nursing Association (JNA) established
the Clinical Nurse Specialist System in 1994 with the
following purpose. Our goal is to contribute to the devel-
opment of health and welfare as well as improving nurs-
ing science by sending CNSs with deepened knowledge
and skills in specic specialized nursing elds to the
society and provide high level nursing care efciently to
individual, families and population with complicated and
intractable nursing issues. The JNA denition of CNS
which named Certied Nurse Specialist is the person
certied as a nurse with excellent nursing practice com-
petency in a specialized eld. CNSs plays the following
six roles:
•
To provide excellent nursing practice to individual,
families and population.
•
To provide consultation to care providers including
nurses.
•
To coordinate among the concerned
multi-disciplinary professions to provide
required care smoothly.
•
To solve ethical issues and conict to protect the
right of individual, families and population.
•
To educate nurses to improve care.
•
To conduct research activity in their clinical settings
to advance and develop professional knowledge
and skills.
There are 13 specialized elds as of 2018; Cancer
Nursing, Psychiatric Mental Health Nursing, Community
Health Nursing, Gerontological Nursing, Child Health
Nursing, Women’s Health Nursing, Chronic Care
Nursing, Critical Care Nursing, Infection Control
Nursing, Family Health Nursing, Home Care Nursing,
Genetics Nursing, Disaster Nursing are identied.
The JNA certies nurses as CNS upon completion of
the CNS curriculum in the master’s programme, and
passing the certicate examination given by JNA. The
title of CNS is protected by trademark registration and
allowed to use it by the nurses who are certied by
JNA. CNSs contribute to improve quality of nursing in
their clinical settings and community by providing not
only direct care but also through consultation, educa-
tion, coordination and ethical coordination to nurses
and multi-disciplinary professions. Moreover, CNSs
contribute to develop efcient care by accumulating
evidence through research (Satomi Sai, Department
of International Affairs, Japanese Nursing Association).
APPENDICES
34 35
Turkey
Specialization in nursing in Turkey was legally dened
in 2007. According to the Nursing Law nurses who com-
pleted their postgraduate education in the eld of nurs-
ing were entitled as specialist nurse. Item 8- ‘Nurses
who have specialized by completing postgraduate pro-
grams related to their profession and whose diplomas
are registered by Ministry of Health and nurses who are
graduates of these programs abroad and whose dip-
lomas are approved as equivalents work as a specialist
nurse.’ (Law No: 6283 RG:2.5.2007/26510). Although
master’s education for the Clinical Specialist Nurse
exists for a long time (from 1960s) their ofcial pos-
ition has not been integrated into healthcare systems.
Until now, the only setting where nurses can use their
specialization areas in in the universities. Recently the
Department of Healthcare Services under the Ministry
of Health called for an action plan to develop criteria/
qualications for the employment of CNS as an ofcial
position. As of 2019 a task force has been assigned
under the Turkish Nurses’ Association to explore this
possibility (Turkish Nursing Association).
United Kingdom (UK) (England, Northern Ireland,
Scotland, and Wales)
The specialist nurse role in the UK started in the 1970s
and has been described as a combination of four elem-
ents: clinical, education, research and consultation. A
study conducted in England, Scotland and Wales found
that the majority of the clinical work of the CNS con-
sisted of physical assessment, referral, symptom con-
trol and ‘rescue’ work. However, it was reported that the
work of the CNS is often invisible because the manage-
ment of patients is through complex care pathways and
oversimplied. As a result, the CNSs act as ‘fail safes’
in preventing injury, detecting symptoms and preventing
sequelae, preventing or dealing with iatrogenic events
and often dealing with issues before they become com-
plaints (Leary et al. 2008). A major issue in the UK is
that most CNSs are not educated at the master’s level
and this has resulted in confusion and inconsistency
in terms of complexity of patient and health systems
issues the CNSs address. The title CNS is not used
consistently in all four UK countries as there is no regu-
lation around the use of this title. Most are highly expert
specialised nurses but not Advanced Practice Nurses
that meet the criteria for a CNS. Lack of title protection,
standardised requirements for education and excessive
workloads present barriers to optimal CNS practice in
the UK (Prostate Cancer UK, 2014).
United States of America (USA)
The American Association of Colleges of Nursing
(AACN) describes CNSs as clinicians who are experts
in evidence-based nursing and practice in a range of
specialty areas, such as oncology, pediatrics, geriatrics,
psychiatric/mental health, adult health, acute/critical
care, and community health among others. In addition
to direct patient care, CNSs also engage in teaching,
mentoring, consulting, research, management and sys-
tems improvement. Able to adapt their practice across
settings, these clinicians greatly inuence outcomes by
providing expert consultation to all care providers and
by implementing improvements in healthcare delivery
systems.
The American Nurses Association’s denition (2004:15)
states that:
Clinical nurse specialists (CNSs) are registered
nurses, who have graduate level nursing
preparation at the master’s or doctoral level as a
CNS. They are clinical experts in evidence-based
nursing practice within a specialty area, treating
and managing the health concerns of patients and
populations. The CNS specialty may be focused
on individuals, populations, settings, type of
care, type of problem, or diagnostic systems
subspecialty. CNSs practice autonomously and
integrate knowledge of disease and medical
treatments into assessment, diagnosis,
and treatment of patients’ illnesses. These
nurses design, implement, and evaluate both
patient‑specic and population‑based
programs of care.
CNSs provide leadership in advancing the practice
of nursing to achieve quality and cost-effective
patient outcomes as well as provide leadership
of multidisciplinary groups in designing and
implementing innovative alternative solutions
that address system problems and/or patient
care issues. In many jurisdictions, CNSs as direct
care providers, perform comprehensive health
assessments, develop differential diagnoses,
and may have prescriptive authority. Prescriptive
authority allows them to provide pharmacologic
and nonpharmacological treatments and order
diagnostic and laboratory tests in addressing and
managing specialty health problems of patients
and populations. The CNS serves as a patient
advocate, consultant, and researcher in various
settings.
Appendix 3: The International Context and Country Examples of the NP
It is beyond the scope of this paper to identify all coun-
tries where NPs are present; however, this appendix
offers exemplars where the NP role is established and
identiable in order to provide examples of established
NP initiatives. In addition, new initiatives with active
support are described to broaden the perspective of
international development. In describing the inuence
of context, it is worth mentioning the unique approach
relevant to Advanced Practice Nursing emerging in
England. The Advanced Nurse Practitioner has become
part of the wider remit of Advanced Clinical Practice
(ACP) which incorporates a wide range of non- medical
healthcare professionals under a framework for the
ACP workforce (HEE 2017).
Australia
In Australia, the NP title is protected and only nurses
who have been authorised by the National Nursing and
Midwifery Registration Board of the Australian Health
Practitioner Regulation Agency may use the NP title.
A master’s level education specic for the NP is the
minimal level of education required to practice. In
2014 (NMBA, updated 2018), the NP standards were
reviewed and the following standards were imple-
mented. The NP: 1) assesses and uses diagnostic
capabilities; 2) plans care and engages others; 3) pre-
scribes and implements therapeutic interventions;
4) evaluates outcomes and improves practice.

GUIDELINES ON ADVANCED PRACTICE NURSING 2020
36
The NP scope of practice is built on the basis of the
registered nurse (RN) scope of practice and must
meet the regulatory and professional requirements for
Australia including the Registered nurse standards for
practice and Code of conduct for nurses. The NP stand-
ards build on and expand upon those required of an
RN. The NP is expected to understand the changes in
scope of practice from the RN and the ways that these
changes affect responsibilities and accountabilities
(NMBA 2018).
Anglophone Africa APN Coalition
Under the title ‘Anglophone Africa Advanced Practice
Nurse Coalition Project (AAAPNC): A Proposal to
WHO (Africa) Health Systems Leadership’ (Sibanda &
Stender, 2018) ve countries have set a priority to initi-
ate Family Nurse Practitioner (FNP) programmes and
to start work on midwifery advanced practice by the
end of 2020. Strong support for this initiative is being
provided by experts and universities in the UK and the
USA. To achieve the aims of the project, the intent is
to instigate robust research developing Afrocentric
models and frameworks relevant to population needs
and healthcare systems. In addition, the intent is to
collaborate with representatives in medicine, phar-
macy and other healthcare disciplines. In a gesture of
support, LeadNurseAfrica dedicated its April 2019 pre-
conference workshops in Ghana to Advanced Practice
Nursing.
African universities that have agreed to participation
in this initiative include: Aga Khan University sites in
Kenya, Uganda and Tanzania already in advanced
stages of the development of MScN (APN) curriculum
in collaboration with the Nursing Council of Kenya;
University of Botswana, the only African institution
with a master’s degree for the FNP that matches inter-
national APN standards in education, accreditation and
regulatory practice; and The School of Nursing and
Midwifery, University of Ghana.
The concept of Advanced Practice Nursing has been
identied in South Africa, Kenya, Zambia, Malawi,
Swaziland, Botswana, Uganda and Rwanda, but the
scope of practice and legislation to formalise their
respective practices are not explicit (Sibanda & Stender
2018) and in most African countries achieving the inter-
national standard of master’s degree education is still
aspirational.
Botswana
Country independence, a need for health care reform
and a shortage of physicians triggered the need for
nurses to accept increased responsibilities for PHC in
Botswana, but the nurses ultimately demanded add-
itional education to accomplish this. The rst Family
Nurse Practitioner (FNP) programme was established
at the Institute of Health Science in 1981 followed by
revisions of the curriculum in 1991, 2001 and 2007.
Candidates must have: 1) a qualied nursing degree,
2) minimum experience of two years as a nurse, 3) be
registered with the Nursing and Advance Diploma in
Midwifery Council of Botswana, and 4) be in posses-
sion of a Botswana General Certicate of Secondary
Education or its equivalent. In addition, the University of
Botswana offers a master’s programme for the FNP with
efforts in process to join components of the two FNP
educational options. Nurse Practitioners in Botswana
provide primary care in outpatient departments, clin-
ics, industrial settings, schools, private practice, and
commonly in nurse/NP managed clinics. Even though
there is success in the country, there is still a need for
stronger policies and regulatory systems to support the
NPs (Seitio-Kgokgwe et al. 2015).
Canada
In Canada, the only Advanced Practice Nursing role with
additional regulation and title protection beyond that of
the generalist nurse is the NP. NPs can autonomously
make a diagnosis, order and interpret diagnostic tests,
prescribe pharmaceuticals and perform specic pro-
cedures within their legislated scope of practice (CNA
2009). The Nurse Practitioner Association of Canada
(2018) offers the following denition:
In Canada, Nurse Practitioners (NPs) are licensed by
jurisdictional nursing regulators. NPs are graduate pre-
pared health care providers who practice autonomously
and independently. NPs provide direct care to patients
to diagnose and manage disease/illness, prescribe
medications, order/interpret laboratory/diagnostic tests
and initiate referrals to specialists.
(NPAC-AIIPC 2018)
Following a federally funded initiative (Canadian NP
Initiative) a framework for the integration and sustain-
ability for the NP role in Canada’s healthcare system
was developed. NPs now practice in a wide variety of
settings and in various models of care. The NP scope
of practice is dened along with a common role descrip-
tions and liability coverage. The country continues to
work to remove federal and legislative barriers for distri-
bution of medical samples, medical forms for disability
claims and workmen’s compensation (CNA, 2016).
Caribbean Region
Following the example of the NP in the USA and
through the assistance of the Pan American Health
Organization and Project Hope, NP education began in
Jamaica in 1977, and in St. Vincent (discontinued 1987)
and the Grenadines. In St Lucia, Dominica, St Vincent
and the Grenadines, NPs have prescriptive authority for
some drugs and practice mainly in PHC settings with
prescriptive authority guided by a specic formulary. In
St. Vincent and the Grenadines and St Lucia, NPs have
the autonomy to develop their own itineraries. As of
2017, 72 NPs in Jamaica provide healthcare services,
mostly in rural areas. Often, they are given pre-signed
scripts and sometimes required to run the clinics alone.
In the Caribbean Region, the role of the NP is clearly
dened. Education for NPs is offered only at University
of the West Indies School of Nursing in Jamaica. The
master’s degree two-year programme is not funded by
the government. Therefore, some nurses are unable
to access the education due to cost incurred. Upon
completion of the programme NPs are given their
job description which outlines their scope of practice.
Monthly work schedules are assigned by the Medical
Ofcer, Senior Public Health Nurse or identied by
the NPs themselves. Continuing education forms the
framework for NPs to update their knowledge base with
seminars held monthly.
APPENDICES
36 37
Even though Jamaica has been the leader in NP edu-
cation and practice in the region, the issue of lack of
legislation continues to pose a challenge. In St. Lucia,
NPs are given a separate registration/licence while
other NPs in the region are required to use their regis-
tered nurse/midwife licence to practice. Amendment of
the Nursing and Midwifery Act is underway in Jamaica
and the Bahamas since 2018. The greatest opposition
is from the medical fraternity (personal communication,
H. McGrath, March 2019).
New Zealand
The rst NP in New Zealand was endorsed in 2001.
Title protection was initially established through trade-
marking, but the trademarking concept is no longer in
effect. In 2015, the Nursing Council of New Zealand
(NCNZ) removed the requirement that restricted NPs to
a specic area of practice and introduced a new more
general scope of practice. NPs in New Zealand must
have: 1) a minimum of four years of clinical experience
prior to entry into an educational programme, 2) com-
plete an approved master’s degree programme that
includes advanced practice and prescribing competen-
cies, 3) pass an assessment against NP competencies
by an approved panel, and 4) register with the NCNZ
(Schober & Green 2018).
Oman
The idea of the Advanced Nurse Practitioner (ANP)
in Oman was inspired by a 2000 meeting of repre-
sentative countries of the World Health Organization-
Eastern Mediterranean Region (WHO-EMRO) focused
on advancing nursing capacity and nurse prescribing.
The primary motivation for the ANP in Oman was a
shortfall of physicians especially in PHC settings both
in number and expertise. In addition, emerging health
problems, increased life expectancy and a desire to
move care closer to the population and deeper into the
community caught the attention of the Ministry of Health
(MOH). The MOH and Directorate of Nursing were also
aware that nurses, out of necessity, in small healthcare
centres were providing services in an extended scope
of practice and beyond the level of their generalised
nursing education. Following a series of situational ana-
lyses by short term WHO consultants and development
of a strategic direction by the Directorate of Nursing
based on recommendations by a multidisciplinary task
force, it was decided to proceed with the APN concept
along with on the job training (OJT) for nurses in health
centres already functioning in an advanced clinical
capacity.
The rst ANP, educated in a USA NP master’s degree
programme, began practice in Oman in 2016. Since
that time, additional nurses have completed pro-
grammes abroad and at Sultan Qaboos University. The
ANPs practice in their eld of expertise and/or teach in
the College of Nursing, SQU. The OJT for nurses prac-
ticing beyond their scope of practice was implemented
in 2017 with 25 nurses enrolled from all governorates
of Oman. Based on this success, the trajectory for
these nurses is to support them from their extended
role based on OJT to progress to the specialist role
(Bachelor in Community Health Nursing) and then to
the ANP role with a focus on family health (personal
communication, M. Al-Maqbali, April 2019).
Republic of Ireland
In Ireland, the Advanced Nurse Practitioner (ANP)
emerged as a result of the Commission of Nursing
report, which recommended this development in 1998
(Government of Ireland 2008). The rst ANP post in
Minor Injury Emergency Care was accredited in 2002
(National Council for the Professional Development of
Nursing and Midwifery, 2008a). Since then, the ANP
presence continues to develop. The intention is to
establish a critical mass of approximately 700 ANPs by
2021, which goes towards the target of 2% of ANPs
within the nursing workforce (Ofce of the Chief Nurse,
Department of Health 2017). To facilitate this develop-
ment, the Nursing and Midwifery Board of Ireland (NMBI)
published National Standards and Requirements for the
Education of ANPs at master’s level at the end of 2017.
Standards and Requirements for prescriptive authority
had already been in place (NMBI 2015a and 2015b).
ANP core competencies in Ireland include: (1) auton-
omy in clinical practice, (2) expert practice, (3) pro-
fessional and clinical leadership, and (4) research
(National Council for the Professional Development
of Nursing and Midwifery 2008b). The title Registered
Advanced Nurse Practitioner (RANP) is protected
through the NMBI.
United Kingdom (UK) (England, Northern Ireland,
Scotland, Wales)
The rst nurses graduated from the Royal College of
Nursing (RCN) Nurse Practitioner programme in 1992
(RCN 2008). The rst 15 students led the way for NPs
who now practice throughout the UK. During the early
formative years as RCN developed an accreditation
system for educational institutions, the rst UK educa-
tional competencies emerged (Barton & Allan 2015).
Those competencies were based on consultancy skills,
disease screening, physical examination, chronic dis-
ease management, minor injury management, health
education and counseling. The RCN competency
framework (2008) provided criteria for new courses with
these baseline competencies establishing a standard
for ANP practice outcomes (Barton & Allan 2015).
Following devolution, the four countries of the UK
(England, Northern Ireland, Scotland, Wales) devel-
oped their own approaches to health and social care
and therefore also to associated workforce policy
regarding Advanced Practice Nursing. As a result, the
NP developed in different ways and educational prepar-
ation ranges from a generic approach to a growing ten-
dency to establish preparation at the master’s degree
level. Despite enthusiasm for the role, regulation for
ANP has not been established in the UK.
There is a move to a wider perspective of Advanced
Clinical Practice (ACP) emerging in the UK since 2017
(HEE, 2017). Identifying with ACP incorporates a wide
range of non-medical healthcare professionals within
the multiprofessional ACP category extending to allied
health professionals. Therefore, use of ‘advanced’ titles
vary within and across institutions. England has taken
this further to include pharmacists and social workers.
In Scotland, there are separate nursing and paramedic
work streams and work has started to widen to other
allied health professionals. The focus in Northern
Ireland is currently nursing but discussions have started
regarding expanding this to allied health professionals
(personal communication, K. Maclaine, 8 March 2019).
GUIDELINES ON ADVANCED PRACTICE NURSING 2020
38
In a September 2018 brieng, the Council of Deans of
Health (2018) in the UK provided a brieng paper to
identify UK country differences:
Wales: A framework for Advanced Nursing,
Midwifery and Allied Health Professionals Practice
in Wales was developed in 2010 and reviewed in
2012. This framework derived content and built on
Scotland’s advanced practice toolkit for nursing
(2008), including the supporting principles. In align-
ment with ACP, Wales has seen the emergence of
many advanced practice roles.
Scotland: Scotland has had an advanced practice
toolkit since 2008 and a framework for Advanced
Nursing Practice since 2012. Scotland has devel-
oped a national approach to Advanced Nurse
Practitioner (ANP) education based on expect-
ations identified in 2017 by the Transforming
Nursing Advanced Practice Group. The country
has a goal to develop an additional 500 Advanced
Nurse Practitioners over the coming years with
funding support of the Scottish Government.
England: The Multi-professional Framework for
Advanced Clinical Practice (ACP), published in
2017, is expected to be implemented in 2020. The
ACP framework sets out an agreed denition of ACP
for health care professionals to work at a higher
level from initial registration. Currently, advanced
practice is not regulated in the UK, therefore Health
Education England (HEE) are developing an
Academy for Advancing Practice for governance of
education and quality of healthcare services.
Northern Ireland: Northern Ireland published an
Advanced Nursing Practice framework in 2014
(NIPEC 2014) to provide clarity about the Advanced
Nurse Practitioner role. The framework is intended
to act as a guide for commissioners, workforce
planners, executive directors of nursing, educa-
tion providers, employers and managers of nurses,
including nurses themselves. Education require-
ment is through a master’s programme including
a non-medical prescribing being an essential com-
ponent. The graduate receives an award title, for
example, an ‘MSc in Advancing Practice Education
in [Profession]’.
Western African Sub-region
The idea of having an APN programme in the Western
African region has been considered for some time but,
as of April 2019, this is still aspirational with proposals
not reaching a logical conclusion (personal communi-
cation, April 2019, O. Irinoye). There was an attempt
to start an APN programme in Nigeria in 2011 work-
ing with stakeholders in Nigeria and the University of
Maryland, USA (Irinoye, 2011). The hope was for three
universities to incorporate the Family Nurse Practitioner
(FNP) Programme into postgraduate programmes. The
initiative has been stalled due to funding issues and
the need to work on policy dimensions for introducing
this new cadre of nurses into the healthcare workforce.
However, discussions have resumed with the intention
to include FNP content into the current revision of the
postgraduate programme to benet nurses who are in
or plan to start private practice.
Appendix 4: Country exemplars of adaptations or variations of CNS and NP
As countries and regions identify and implement
Advanced Practice Nursing the evolution of these roles
or levels of nursing are not always specic to CNS or
NP. Sometimes the approach is seen as a blended role
of CNS and NP, in other instances language translation
or healthcare culture inuences the portrayed perspec-
tive of Advanced Practice Nursing and the APN. This
appendix provides exemplars of this variance.
Germany
The situation in Germany is complex while progress-
ing with Advanced Practice Nursing. There are nursing
councils in isolated federal states with the process under
construction since 2016. The challenges for German
APNs include problems for registration, title protection
and autonomy. Since 2000 to the present time there
are model projects and concepts in individual clinics
for APNs. Opportunities for study programmes in vari-
ous cities in Germany are steadily increasing. Position
papers from nursing associations have supported the
role. The German Council of Economic Experts has
called for care to be implemented on an evidence-based
level. In addition, the advice is given that nursing care
should be taken in the context of the assessment of
popu lation needs (personal communication March 2019,
S. Pelz, S. Inkrot, A. Schmitt, C. von Dach).
Hong Kong
In Hong Kong, the Hospital Authority of Hong Kong
introduced the nurse specialist role in 1994, then
changed the title classication to APN in 2000 and then
subsequently established an advanced rank position of
Nurse Consultants in 2009 to facilitate these nurses to
make greater impacts on services at system level. The
Hospital Authority is the healthcare provider in the pub-
lic sector. Hong Kong also has a large private health-
care sector where nurses provide services using their
advanced competencies to serve clients in different
specialties and settings.
The Hong Kong Academy of Nursing is formed, led by
nurse leaders in Hong Kong, from both public and private
sectors. The Academy, representing essentially all spe-
cialties in practice, has a system in place to accredit the
Academy Colleges and certify members and fellows who
fulll the curriculum and clinical experience requirements
and have passed examinations at the advanced practice
level. The Government of Hong Kong in 2018 instructed
the Nursing Council of Hong Kong to set up a group to
make a proposal on scope of practice, core competencies
and training mechanisms for an advanced practice regis-
ter under the Nursing Council. The scheme will initially
be on a voluntary basis and will then be considered by
the government to convert it into a statutory registration
regime (personal communication, F. Wong, March 2019).
The Netherlands
In the Netherlands, Advanced Practice Nursing is a com-
bination of the role of the NP in direct patient care, and of the
CNS in being a leader in nursing, for example by improv-
ing the quality of healthcare, by doing scientic research
and by enhancing the quality of the professional care team
(personal communication, March 2019, Ms. I.H. de Hoop,
President Dutch Nurse Practitioner Association).

APPENDICES
38 39
In 1997, the role was an initiative of a hospital, the
University Medical Center in Groningen to improve
nursing care at an advanced level. A new healthcare act
ended the act that prohibited medical care by nonphys-
icians. This opened the possibilities to create a position
for nurses to provide complex healthcare services for
a well-dened group of patients to improve continuity
of care. The rst master’s programme at the Hanze
University of Applied Science commenced at the end
of 1997 with 16 students using a USA programme as
a model. The vision of the APN gained strength and
within a few years nine universities of applied science
offered the master’s programme combining theory and
practice (P.F. Roodbol in Schober, 2017). Development
from 1997 to 2019 is largely due to support from the
Dutch government.
Even though the concept of ‘Nurse Practitioner’ was
known in the Netherlands, the title was not translatable
to Dutch thus the title NP was not protected, therefore
the only possibility in the law was to establish legis-
lation for specialisation. Using the title ‘nurse special-
ist’ in Dutch, it became possible to protect the title and
establish a registration process. Title protection allowed
for identication of the role with the consequence of
malpractice removal from the register with no possi-
bilities to continue to practice if a nurse misrepresents
his or her position in the healthcare system. Factors
that have promoted progress in the Netherlands are
a clear denition of Advanced Practice Nursing, legal
registration (title protection) and credentialing to offer
safe and responsible care and cure (P.F. Roodbol in
Schober 2017). As of February 2016, approximately
2,750 nurse specialists have been educated and regis-
tered in the country. The shortage of physicians that
prompted the introduction of the role in the Netherlands
has been resolved, but the numbers of nurse special-
ists continue to increase. These nurses are accepted
as a professional that provides high quality care and
friendly advice (J. Peters in Schober & Green 2018).
Singapore
The Advanced Practice Nurse (APN) is a protected title
in Singapore, and the APN role is a hybrid of the NP
and CNS role. The National University of Singapore
(NUS), under the auspices of the Yong Loo Lin School
of Medicine, established the master of nursing pro-
gramme in 2003. Since then, this is the only programme
accredited by the Singapore Nursing Board (SNB) to
provide APN education, and it is a pre-requisite for APN
certication. The programme initially offered academic
preparation in adult health and mental health. In 2009,
offerings were extended to a critical care track and sub-
sequently a pediatric track was offered in 2012.
Following completion of a two-year master’s pro-
gramme, graduates must complete a minimum of a
one-year structured internship and pass the national
licensing examination, objective structured clinical
examination (OSCE), before applying for APN certi-
cation, licensure and registration with the Singapore
Nursing Board (SNB). All APNs must meet minimum
clinical practicum hours and achieve required CNE
points for annual renewal of their APN practice licenses
with SNB.
SNB details the APN scope of practice and core com-
petencies for APNs. The core competencies are organ-
ised into four domains. They are professional, legal and
ethical nursing practice; management of care; leader-
ship and management; and professional development.
Each competency domain has associated competency
standards, with each standard representing a major
function/functional area to be performed by an APN.
In 2018, the Singapore Ministry of Health, NUS Alice
Lee Centre for Nursing Studies and the NUS pharmacy
department co-developed and co-hosted the three-
month national collaborative prescribing programme
(NCPP) to prepare APNs and pharmacists for pre-
scribing under a Collaborative Practice Agreement with
medical practitioners. The programme is offered twice
a year. As of April 2019, 74 APNs and pharmacists
have completed the programme, and received or were
waiting to receive the authority licenses to prescribe
medications without the requirement of physician sig-
natures (www.pharmacy.nus.edu.sg/national-collabora-
tive -prescribing/) (personal communication April 2019,
Zhou Wentao, NUS Programme Director (Master of
Nursing).

